Arterial Thoracic Outlet Syndrome Causing Basilar Artery Ischemic Stroke
Mermelstein Maor1*, Belenky Alexander2,5, Shaked Einat3, Sivak Galit4,5, Barnea Rani1,5, Raphaeli Guy1,5, Auriel Eitan1,5 and Peretz Shlomi1
1 Department of Neurology, Rabin Medical Center, Israel
2 Department of Imaging, Rabin Medical Center, Israel
3 Department of Neurology, Sheba Medical Center, Israel
4 Department of Vascular Surgery, Rabinc Medical Center, Israel
5 Department of Medicine, University of Tel- Aviv, Israel
- *Corresponding Author:
- Mermelstein Maor
Department of Neurology,
Rabin Medical Center,39 Jabotinski St.,
Petah
Tikva 49100,
Israel,
Tel : +972-3-9376358;
Email: maorme1@clalit.org.il
Received Date: October 13, 2021;Accepted Date: October 27, 2021;Published Date: November 03, 2021
Citation: Mermelstein M, Belenky A, Shaked E, Sivak G, Barnea R, et al. (2021) Arterial Thoracic outlet syndrome causing basilar artery ischemic stroke. Neurol. Sci. Vol.5 No: 5.08.
Abstract
Introduction: We present here a case of a young woman with sub-acute arterial thoracic outlet syndrome (aTOS) and an acute presentation of basilar artery ischemic stroke. A TOS is a rare subtype which accounts for 1% of TOS spectrum and is almost always associated with a bone anomaly.
Case report: A 29-year-old patient presented with acute stroke and concurrent sub-acute occlusion of her right brachial artery. Investigation for stroke in the young was negative for cardio-embolic source, hyper-coagulability, occult malignancy and large vessel vacuities. Revision of the CT angiography revealed a rib cage bone anomaly in the form of right first and second rib synostosis causing a compression of the right subclavian artery. A TOS diagnosis was made based on clinical symptoms, CTA imaging and a positive dynamic arm duplex ultrasound evaluation. In the absence of an alternative etiology – basilar artery occlusion was presumed to result from retrograde thromboembolism originating in the diseased subclavian artery. Thoracic outlet decompression surgery was performed for both treatment of limb ischemia and prevention of recurrent stroke.
Discussion: Dozens of cases associating aTOS and ischemic stroke have been reported. All cases showed a bony deformity causing stenosis and post-stenotic aneurysm of the subclavian artery, predisposing to thrombosis. Retrograde embolization might occur during dynamic arm movements and transient retrograde flow. Propagation of the thrombus to cervical arteries is an alternative explanation.
Conclusion: Our case highlights the importance of aTOS as a treatable cause of idiopathic stroke in the young, particularly when preceded by symptoms of upper limb ischemia. When diagnosed, patient may benefit from secondary stroke prevention by surgery.
Keywords
Thoracic outlet syndrome; Stroke in the young; Ischemic Stroke; Rib cage abnormalities
Introduction
Thoracic outlet syndrome (TOS) refers to a spectrum of signs and symptoms that are caused by compression of the neuro- vascular organs in the confined space of the thoracic outlet [1]. The rarest presentation is of arterial TOS (aTOS) subtype, which accounts for 1% of cases. The arterial compression can cause distal thromboembolism, arm claudication, or acute arterial ischemia [2]. A higher incidence of bony anomalies is found is patients with TOS, and about 8.5% of all TOS cases are due to a cervical rib [3]. The subtype of aTOS is almost always associated with a bone anomaly (>90%). Diagnosis is made based on clinical presentation and imaging such as duplex ultrasonography, CTA, MRI and conventional angiography [4].
We present here a case of a young woman with sub-acute aTOS and an acute presentation of basilar artery ischemic stroke.
Case Presentation
The patient was a 29 Years old female, left dominant, medical history was notable for heavy smoking, drug abuse, several suicidal attempts and bi-polar disease.
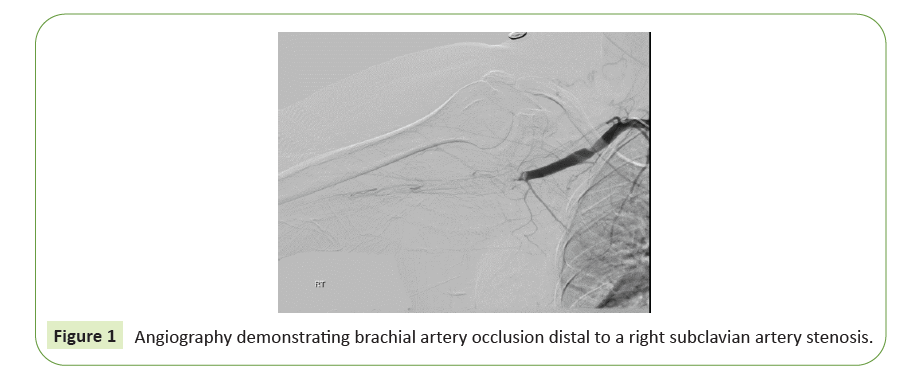
The patient was first admitted to another hospital presenting with sudden loss of consciousness and was diagnosed with acute basilar artery occlusion and extensive pontine infarct. Thrombectomy was preformed successfully but with distal embolization to the P2 segment of left PCA. Patient was admitted to the intensive care unit where she was first noted to have a cold, pale and pulseless right hand. Patient's family reported that the right hand had been cold for several weeks but seemed more severe at that moment. CTA demonstrated compression on the Right Subclavian Artery between the first rib and the clavicle (this effect was suspected to be positional), a filling defect in the right subclavian artery distal to the origin of the vertebral artery and complete occlusion of the brachial artery. Emergent surgical thrombectomy and subsequent attempts at angiography failed to achieve recanalization (Figure 1). Patient was treated with full dose LWMH. Work-up included trans-esophageal echocardiography, Holter ECG and a full battery for hypercoagulability without significant findings. Patient was discharged to an in-patient rehabilitation unit with anarthria and severe tetra-paresis.
Several weeks later, patient referred to our medical center with symptoms of right visual field disturbances, headache, vertigo and vomiting. Physical examination exhibited dysarthria and dysphonia, right homonymous hemianopia and spastic tetraparesis. Head CT, CTA and diffusion-weighted MRI did not show acute pathology. The filling defect in the right subclavian artery remained unchanged. Further workup included a normal EEG, and a negative PET-CT scan which was performed to exclude Takayasu arteritis or another active large vessel vasculitis.
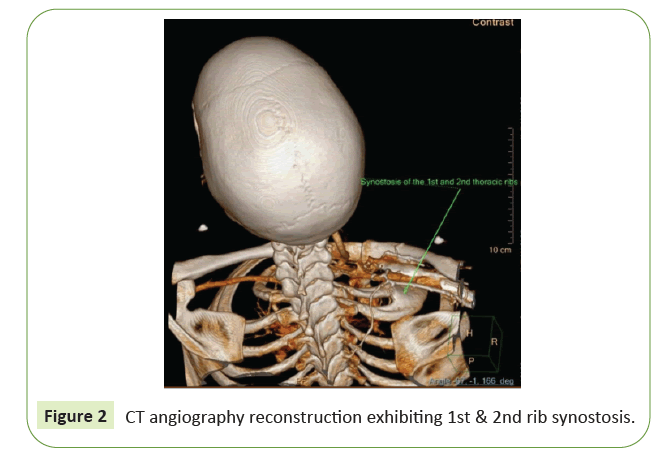
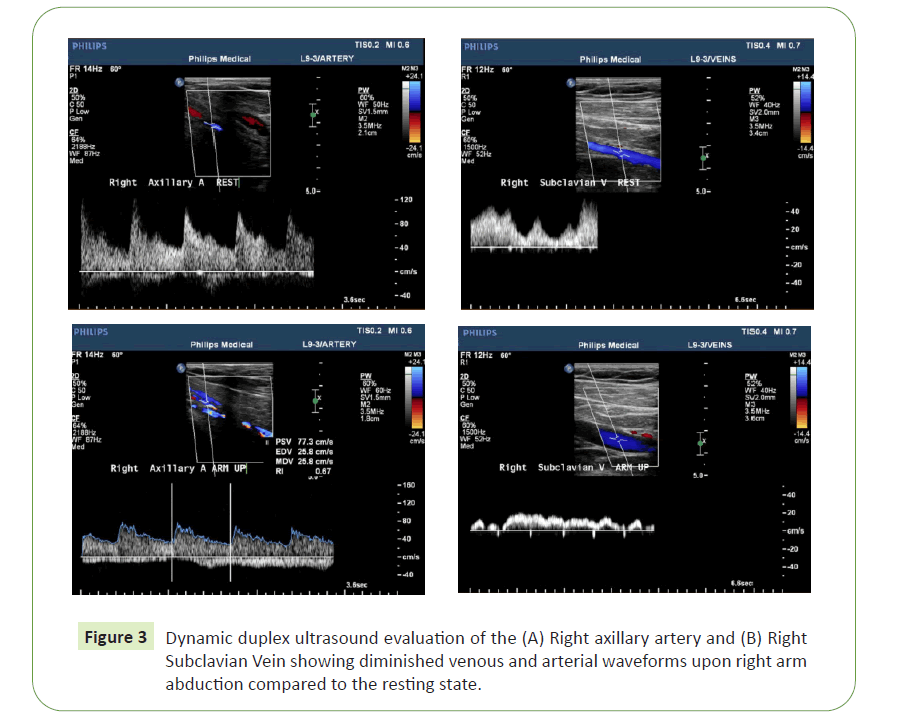
Revision of the patient's imaging revealed a rib cage bone anomaly in the form of a congenital right first and second rib synostosis causing a compression of the subclavian artery between the hypertrophied synostotic ribs and the clavicle (Figure 2). Dynamic duplex ultrasound evaluation of the subclavian and axillary artery and vein showed diminished venous and arterial waveforms upon right arm abduction compared to the resting state (Figure 3). An evaluation of the left arm did not demonstrate such an effect. Based on these unique imaging findings in combination with clinical symptoms of right arm ischemia in relation to arm extension and exertion, a diagnosis of right a TOS was made. In the absence of an alternative etiology, basilar occlusion was presumed to result from retrograde thromboembolism originating in the diseased subclavian artery.
Our patient underwent open decompressive surgery with resection of the first thoracic rib and repair of the right subclavian artery. Her neurological status continued to improve, and she was able to walk on her own. No further ischemic events occurred during follow-up.
Discussion
A review of the literature reveals dozens of cases associating aTOS and ischemic stroke, dating back to 1927 [5].
Several pathogenic explanations for this association have been suggested. Impression of the bone on the subclavian artery causes a stenosis and, in some cases, a post-stenotic dilation and aneurysm due to turbulent flow. The degree of stenosis changes with arm posture and may reach complete occlusion. This can be demonstrated by dynamic angiography or duplex ultrasound. In a post-stenotic aneurysm, thrombosis might evolve and lead to anterograde upper limb emboli or ischemia. Alternatively, when the arm is abducted, severe stenosis or occlusion may cause transient retrograde flow, causing thrombus to dislodge and travel into the vertebral or carotid arteries, resulting in ischemic stroke. Another proposed theory is retrograde propagation of the thrombus through a cervical artery causing a stroke.
These theories are supported by epidemiological data. In all reported cases involving a TOS and carotid artery territory strokes, the bone deformity was ipsilateral to the ischemic hemisphere. Furthermore, in a review of 19 published cases of stroke with associated cervical rib, all 12 cases with anterior circulation strokes involved a right-sided cervical rib [6]. This probably reflects proximity of the origin of the right common carotid artery from the innominate artery to the aTOS stenotic site in the right subclavian artery. In contrast, retrograde embolization or propagation of thrombus from the left subclavian artery to the left common carotid artery which originates separately from the aortic arch is highly unlikely and, indeed, has never been described. The seven posterior circulation strokes reported in t6he review were still mainly right-sided (five out of seven), possibly owing to over-exertion of the right hand in more prevalent right side-dominant patients or to other anatomical factors still not properly elucidated.
A TOS is highly associated with bone anomalies, most commonly with a cervical rib. However, reports on synostosis of the first and second ribs as a cause of aTOS, as in our case, are sparse. Whereas a cervical rib can be readily identified in a simple chest radiograph, the identification of synostosis is more challenging, usually requiring computed tomography and a careful inspection of the imaging data.
Conclusion
Our case highlights again the importance of aTOS as a treatable cause of idiopathic stroke in the young. Particularly, it should be suspected when ischemic stroke is preceded by symptoms of upper limb ischemia. When diagnosed, patient may benefit from surgical decompression for secondary prevention of a potentially devastating ischemic stroke.
References
- Sanders RJ, Hammond SL, Rao NM (2007) Diagnosis of thoracic outlet syndrome. J Vasc Surg.46:601-604.
- Hood DB1, Kuehne J, Yellin AE, Weaver FA(1997) Vascular complications of thoracic outlet syndrome. Am Surg.63:913-7.
- Cormier JM, Amrane M, et al., (1989) Arterial complications of the thoracic outlet syndrome: fifty-five operative cases. J Vasc Surg.9:778-87.
- Henry BM, Vikse J, Sanna B, et al.,(2018) Cervical Rib Prevalence and its Association with Thoracic Outlet Syndrome: A Meta-Analysis of 141 Studies with Surgical Considerations. World Neurosurg.110:e965-e978.
- Palmer OP, Weaver FA(2015)Bilateral cervical ribs causing cerebellar stroke and arterial thoracic outlet syndrome: A case report and review of the literature. Ann Vasc Surg.29:840.e1-840.e4.
- Symonds CP(1927) Two cases of thrombosis of subclavian artery with contralateral hemiplegia of sudden onset, probably embolic.Brain.50:259-60.
Open Access Journals
- Aquaculture & Veterinary Science
- Chemistry & Chemical Sciences
- Clinical Sciences
- Engineering
- General Science
- Genetics & Molecular Biology
- Health Care & Nursing
- Immunology & Microbiology
- Materials Science
- Mathematics & Physics
- Medical Sciences
- Neurology & Psychiatry
- Oncology & Cancer Science
- Pharmaceutical Sciences