Complex Radiological Findings in Congenital Pseudarthrosis of the Tibia
1Laboratory of Radiology, Russian Ilizarov Scientific Centre, Kurgan, Russia
2Faculty of Trauma and Orthopaedics, Tyumen State Medical University, Tyumen, Russia
3Department of Trauma Orthopaedic, Russian Ilizarov Scientific Centre, Kurgan, Russia
- *Corresponding Author:
- Diachkova Galina
Head of Laboratory of Radiology, Russian
Ilizarov Scientific Centre, Kurgan, Russia
Tel: +7 3522 45-26-14
E-mail: dgv2003@list.ru
Received date: November 01, 2018; Accepted date: December 20, 2018; Published date: December 26, 2018
Citation: Galina D, Diachkov KA, Borzunov D, Kutikov SA (2018) Complex Radiological findings in Congenital Pseudarthrosis of the Tibia. J Orthop Disord Vol.1: No.1:5.
Abstract
Objective: To study changes of bone and soft tissues in patients with congenital pseudoarthrosis by MSCT and MRI. Methods: We studied condition of bone and soft tissues at the site of congenital pseudoarthrosis of the tibia before commencing treatment, using radiographic methods- multi slice computed tomography (MSCT), magnetic resonance imaging (MRI) in order to make prognosis of treatment outcome and recurrence of the disease. Results: 25 patients with congenital pseudoarthrosis of the tibia (CPT) in the age group 8 to 40 years were examined by above mentioned radiographic methods, multi slice computed tomography (MSCT), magnetic resonance imaging (MRI) before treatment and after recurrence. The peculiarities and changes in structure of tibial and fibular cortex, periosteum and muscles at the site of pseudoarthrosis. We derived at complex findings and changes that cause recurrence, of pseudarthrosis after deformity correction, or treatment. We developed criteria for evaluation of bone quality in patients with CPT. Conclusion: Structural changes in the soft tissue and the bone at the site of CPT, detected by MRI and MSCT, allow for rather precise interpretation of condition of bone, periosteum, muscles during various stages of treatment and this information can be used to choose appropriate technique and methods of treatment. Keywords: Pseudarthrosis; Tibia; Multi Slice Computed Tomography (MSCT); Magnetic Resonance Imaging (MRI) Key Points • Use of MSCT and MRI for study of pseudoarthrosis made it possible to determine complex changes of bone and soft tissues. • Changes of the tibia in patients with CPT were described as “Complex changes of CPT”. • Criteria for evaluation of bone quality in patients with CPT were introduced
Keywords
Pseudarthrosis; Tibia; Multi Slice Computed Tomography (MSCT); Magnetic Resonance Imaging (MRI)
Key Points
• Use of MSCT and MRI for study of pseudoarthrosis made it possible to determine complex changes of bone and soft tissues.
• Changes of the tibia in patients with CPT were described as “Complex changes of CPT”.
• Criteria for evaluation of bone quality in patients with CPT were introduced.
Introduction
Congenital pseudoarthrosis of the tibia (CPT) remains one of the most complicated and rare condition, and this pathology still remains the subject of focus for many specialists, because complicated long and multi-stage surgical treatment and poor outcomes in 20-50% of cases [1-7]. Indisputable success was achieved in reconstructive and restorative surgical treatment of CPT but orthopaedic surgeons are still not satisfied with longterm results of rehabilitation and high risk of recurrence [8-12]. Efficiency of new methods of treatment (bone morphogenetic protein, stromal cell bone marrow grafts, induced membrane technique) still requires confirmation [13-23]. According to the literature neurofibromatosis type I, occurs only in 40-55% of congenital pseudoarthrosis cases and cannot be considered the only cause of the disease [24-26]. According to data of some authors, the cause of obstinate bone defect at the site of pseudoarthrosis is osteolytic activity of thickened periosteum with pathological structure [27-30]. According to morphological studies of Cho et al. cell contents at the site of congenital pseudarthrosis (fibrous hamartoma) is supported by several mesenchymal phenotypes of cell line; and osteoblasts are not differentiated under influence of bone morphogenetic proteins (BMP) [31]. It is very important to understand bone quality at the site of CPT; however, it should be more important to understand the degree and extension of the pathologic process in CPT and other conditions before the surgery. Only the method of multi slice computed tomography (MSCT) and magnetic resonance imaging (MRI) make it is possible to study character of bone, periosteum and muscles before surgical intervention [32-39]. Limited works on modern radiographic diagnostic methods of CPT do not allow us to evaluate the role and contribution of MSCT and MRI into solving the problem of CPT recurrence [40].
Materials and Methods
Subjects
The work is based on the study of results of treatment and examination of 25 patients with CPT, among them 11 were females, 14–males. In 93% of patients CPT was located in the lower third of the tibia. In most of the cases, etiology of CPT was associated with neurofibromatosis type 1 (46%), in 23%-fibrous dysplasia and in 31%-was idiopathic. In one case the pseudoarthrosis was located at two levels; in another case location of CPT was on bilateral limbs. Various tibial deformities were present in all patients (procurvatum–115 ± 38°, vs. deformity–154 ± 27°). Only 13% of patients could bear weight on the affected limb. Average shortening of the segment by the time of beginning of treatment at RISC “RTO” was 7.4 ± 4.2 cm. In 89.1% of cases CPT was referred to type IV by Crawford [41]. Before admission to hospital 12 patients underwent single surgery (27%). 11 patients underwent two to five surgeries. Two patients underwent six to eight surgeries, prior to the treatment at RISC “RTO”.
Methods of treatment
The main goal of treatment of CPT was restoration of anatomic and functional capabilities of the affected limb. The patients underwent four types of osteosynthesis. Group-I- monolocal compression osteosynthesis with Ilizarov fixator, without lengthening of the segment was done in 7 patients. Group- II bilocal compression-distraction osteosynthesis with simultaneous lengthening of the proximal fragment in 6 patients. Group-III a combination of Ilizarov fixator and intramedullary osteosynthesis in 5 patients. Group-IV were treated using technology combining the method of inductive membrane Masquelet and Ilizarov bone transport. Analysis of treatment results of patients with CPT indicates that Ilizarov technique of transosseous osteosynthesis in combination with intramedullary osteosynthesis provides more reliable clinical result.
Methods of examination
Radiography: Radiography of the tibia was done in 25 patients with congenital pseudoarthrosis of the tibia (CPT) ranging in age from 8 to 40 years before and after treatment and after recurrence.
Сomputed tomography: The studies were performed using computer tomographs GE Lihgt Speed VCT (GE Medical Systems, Wisconsin, USA), Toshiba Aquilion-64 (Toshiba Medical Systems corporation, Otawara, Toshigi 324-8550, Japan). The study began with the topogram of the segment in AP view. Processing of axial slices was done in the mode of multiplanar reconstruction in frontal and sagittal planes. We studied peculiarities of roentgenmorphology and conducted quantitative evaluation of indices of tibial and fibular density at the site of pseudoarthrosis in Hounsfield units (HU). We performed analysis of topographicanatomic changes in mode 3D-reconstruction with bone and soft-tissue filters of working stations.
Magnetic resonance imaging: 20 patients were examined by MRI method. The study was done on MRI tomograph MAGNETON Symphony syngo MR 1.5 Тс (SIEMENS AG, Munchen, Germany). The study was done in the mode T2 tse (in coronal plane), T2 tse fs (in coronal plane), Т1 fl 2d (coronal plane), T1 se (sagittal plane).
Statistical processing of results
For statistical analysis we used statistic software Attestat. Mean value and standard deviation were calculated for indices of density in the distal part of the tibia in patients with recurrences and without recurrences. Student t-test was used to calculate the value of differences in density in two groups of patients. Critical level of significance when checking statistical hypotheses was equal to р<0.05, where р–level of significance of these criteria. All results were represented as M ± σ, where М – sample average, σ- sample standard deviation [42].
Results
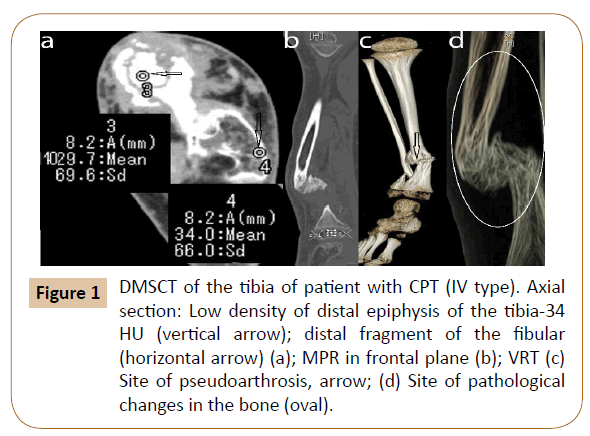
Roentgenography, MSCT, MRI were used to study structure (architecture) of bone at the site of pseudoarthrosis. Roentgenography data was used to classify the pseudoarthrosis and study its location, bone deformity and condition of adjacent joints. MSCT allowed us to reveal fine structural changes in the site of pseudoarthrosis, determine bone density, condition of cortex, its thickness. According to MRI data, the thickness of the periosteum and muscles was measured, and the state of the bone marrow was assessed. The study allowed us to divide the patients into groups according to Crawford, 1986. The most severe changes with deformity, pathological fracture, pseudoarthrosis, affected tibia and fibula were observed in 23 patients (type IV) (Figure 1).
Figure 1: DMSCT of the tibia of patient with CPT (IV type). Axial section: Low density of distal epiphysis of the tibia-34 HU (vertical arrow); distal fragment of the fibular (horizontal arrow) (a); MPR in frontal plane (b); VRT (c) Site of pseudoarthrosis, arrow; (d) Site of pathological changes in the bone (oval).
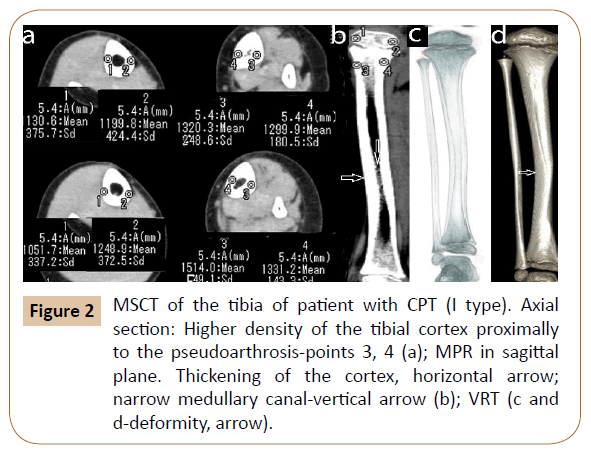
In two patients the changes were referred to type I (deformity of the tibia with increase of cortical layer density) and type II– (deformity with narrow sclerotic marrow canal) (Figure 2).
Figure 2: MSCT of the tibia of patient with CPT (I type). Axial section: Higher density of the tibial cortex proximally to the pseudoarthrosis-points 3, 4 (a); MPR in sagittal plane. Thickening of the cortex, horizontal arrow; narrow medullary canal-vertical arrow (b); VRT (c and d-deformity, arrow).
MRI showed diffuse swelling of soft tissues, hypotrophy of muscles on the anterior surface, thickening of the periosteum, narrowed medullary canal with changed signals. Study of axial sections in patients with CPT in the area adjacent to the pseudoarthrosis showed in the majority of cases thickening of the cortex, narrowing of the medullary canal, its eburnation. MRI visualized soft tissue structures at the site of pseudoarthrosis. In case of significant shortening of the tibia the soft tissues were deformed.
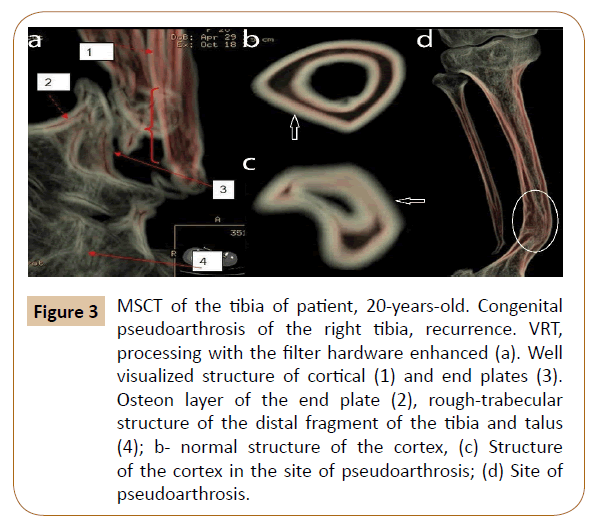
Use of special processing of the work station revealed structure of cortex of the tibia and end plates at the site of the pseudoarthrosis, which were not quite clearly visualized on regular axial slices or MPR. The applied technique of data processing allowed us to visualize the osteon layer, which had smaller thickness and was not visualized over the length of 2.5-4.5 cm. There were thickened bone trabeculae, irregularly positioned in the site of distal epiphysis and talus. The cortex on the border with the pseudoarthrosis was deformed and it did not have clear threezone structure (Figure 3).
Figure 3: MSCT of the tibia of patient, 20-years-old. Congenital pseudoarthrosis of the right tibia, recurrence. VRT, processing with the filter hardware enhanced (а). Well visualized structure of cortical (1) and end plates (3). Osteon layer of the end plate (2), rough-trabecular structure of the distal fragment of the tibia and talus (4); b- normal structure of the cortex, (c) Structure of the cortex in the site of pseudoarthrosis; (d) Site of pseudoarthrosis.
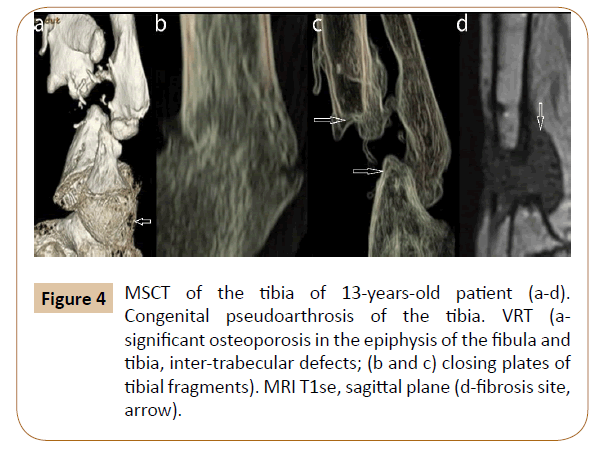
Distal third of the tibia and fibula were deformed; medullary canal of the tibia was not visible and was filled up with bone tissue coinciding in density with the osteon layer of the cortex. Density of the tibia at the site of sclerotic fragments forming the pseudoarthrosis varied significantly (from 1292 to 1976 HU). It is associated with the varying trabecular structure in this site; it can be clearly seen in the MPR and VRT. The most significant changes of architecture of the bone, in parts adjacent to the part forming the pseudoarthrosis were characteristic in patients with repeated recurrence of CPT. Significant structural disorders were observed along with significant anatomic changes. Architecture of the distal fragment was significantly changed. Cortex at some of the involed sites was not formed and did not have clear borders. Use of MSCT allowed us to receive preoperative data on anatomical and structural characteristics of bone in the site of pseudoarthrosis (Figure 4). Resorption sites were clearly visualized as a peculiar “lacelike” picture, indicating intertrabecular defects.
Figure 4: MSCT of the tibia of 13-years-old patient (a-d). Congenital pseudoarthrosis of the tibia. VRT (а-significant osteoporosis in the epiphysis of the fibula and tibia, inter-trabecular defects; (b and c) closing plates of tibial fragments). MRI T1se, sagittal plane (d-fibrosis site, arrow).
Density of the cortex of the three patients in the distal third of the tibia was decreased, there were sites of resorption; it was confirmed by experimental data W. Wang, 2011 in modelling neurofibromatosis I type (NF1).
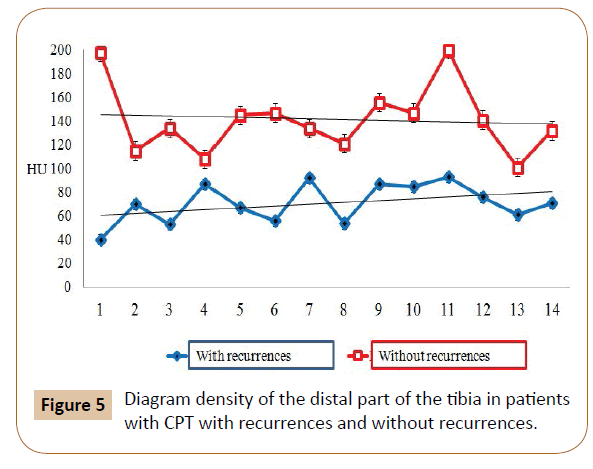
Density of bone in the distal meta-epiphysis, adjacent to the pseudoarthrosis in the three patients was decreased to 30-70 HU, in other patients it was higher (120, 45 ± 24,71 HU). In certain sites of metaphysis there was increase of density up to 214.11 ± 41.75 HU (Figure 5).
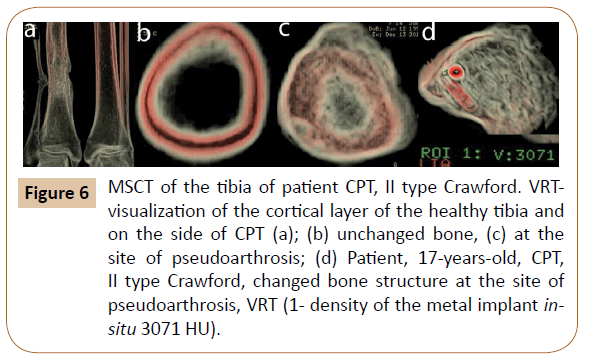
Study of density and structure of the cortex in the site adjacent to CPT showed that it did not have characteristic structure, was thickened, with unclear contours and absence of osteon layer in the majority of cases. Medullary canal was absent in three patients and was filled up with bone structures of various density (Figure 6).
Figure 6: MSCT of the tibia of patient CPT, II type Crawford. VRTvisualization of the cortical layer of the healthy tibia and on the side of CPT (a); (b) unchanged bone, (c) at the site of pseudoarthrosis; (d) Patient, 17-years-old, CPT, II type Crawford, changed bone structure at the site of pseudoarthrosis, VRT (1- density of the metal implant insitu 3071 HU).
For this purpose, criteria for evaluation of bone quality in patients with CPT were introduced (considering changes in the site of pseudoarthrosis) (Table 1).
| Indices of bone quality evaluation | Criteria for bone quality evaluation | ||
|---|---|---|---|
| K1 | K2 | K3 | |
| Crawford type | II | III | IV |
| Condition of bone marrow canal | Narrowed | Narrowed, eburnation | Bone marrow canal is filled up with bone and fibrous structures of various density |
| Structure of the cortex | Thickened | Thickened, endosteum contours are unclear in some places | Thickened, endosteum contours are unclear, osteon layer is absent |
| Extension (mm) of disorder of the cortex structure | 30 | 40 | 50 |
| Density of the cortex at the site of pseudoarthrosis | 1200-1300 HU | 900-1100 HU | 700-900 HU |
| Density and architectonics of the tibia in the distal part | Moderately decreased 150-170 HU Extensive sites of resorption |
Significantly decreased 110-150 HU Complete breakdown of organotypic structure | Very much decreased 60-110 HU Cluster of bones forming the ankle joint |
| Talus density | 95-120 HU | Significantly decreased 85-90 HU | Very much decreased <85 HU |
| Density and architectonics of calcaneus | Partial preservation of arcades, sites of resorption. Body: 160-240, calcaneal tuber 30- 40 HU | Absence of two types of arcades, sites of resorption. | Complete breakdown of organotypic structure |
Table 1: Evaluation of bone quality at the site of pseudoarthrosis according to MSCT data.
Discussion
Use of MSCT and MRI for study of pseudoarthrosis before treatment and after recurrence allowed us to observe anatomic changes (deformity, shortening) of the cortex, medulary canal, adjacent parts of the tibia and fibula, condition of periosteum. Fibrous tissue observed at the site of pseudoarthrosis and changed structure of periosteum was undoubtedly, the key to the pathology, possibly, due to decrease of osteogenic potential and disorders of local vascularization. According to MRI all patients in the site of pseudoarthrosis had formation of hamartoma (site of fibrosis varying in size) and thickening of periosteum. The role of periosteum in pathogenesis of congenital pseudoarthrosis is not quite clear but considering data about increased osteolytic activity of periosteum and disorder of its morphological structure it is possible to suppose its role in pathogenesis of pseudoarthrosis. Morphological study of the resected parts of the pseudoarthrosis resulted in revealing such disorders as «active osteoclastic resorption of the cortex, which remodelled into a trabecular rather than, not compact type of structure», presence of immature bone structures with foci of necrobiosis and necrosis, and also inadequate development of capillary vessels According to MSCT, structure of the cortical plate in the pseudoarthrosis does not contain osteon layer and density of the bone is lower than normal values, especially in patients with recurrences. Electron microscopy data did not show significant structural differences of bone and surrounding soft tissues between CPT secondary to neurofibromatosis I type, fibrous dysplasia and idiopathic form of pseudoarthrosis [43-45]. We also did not observe principal differences in changes of bone and soft tissues in various etiologies of CPT either; those depended more on the number of recurrences and previous surgeries. There is no doubt that our more detailed study of bone structural changes makes contribution into revealing decrease of reparative abilities of tibia and fibula during treatment of CPT. Described changes in the distal part of the tibia in patients with CPT can be combined into the concept of “complex of findings of CPT”, which, depending on the severity of the components, allow us to assess the quality of the bone at the site of pseudoarthrosis to predict the results of treatment.
Conclusion
In conclusion, modern radiographic diagnostic methods allowed us to observe and study maximum possible variants, of anatomic and structural properties of the tibia in patients with congenital pseudoarthrosis. Possibility of in vivo study of bones and soft tissues of the tibia plays the important role. Sclerotic bone fragments, narrow medullary canal or its eburnation, absence of osteon layer in the structure of the cortex, extensive area of fibrosis surrounding the site of pseudoarthrosis, changes of soft tissues explain decrease of osteoblastic potential.
It is necessary to take into account MSCT and MRI data when choosing technique of treatment and planning the surgery for patients with CPT:
1. MSCT: Disorder of three-zone structure of the cortex; amount of tibial shortening, density of distal and proximal fragments of tibia (HU); character and extension of pathological bone remodelling in the distal fragment; character and manifestation of foot bone changes.
2. MRI: Extension and degree of thickening of the periosteum in the distal and proximal fragments; amount of fibrous changes of soft tissues in the pseudoarthrosis site; condition of soft tissues on the anterior surface of the tibia in obvious procurvation deformity; amount of tibial shortening, degree of muscle atrophy; extension of diffuse swelling of soft tissues.
The obtained data makes it possible to determine the extension of resection of the bone fragments, periosteum, feasible amount of lengthening, technique of fixation of bones forming the ankle, need for bone plasty and other techniques for stimulation of bone consolidation in the site of pseudoarthrosis, additional means of fixation (half-pins, wires).
References
- Heikkinen ES, Poyhonen MH, Kinnunen PK, Seppänen UI (1999) Congenital pseudarthrosis of the tibia: Treatment and outcome at skeletal maturity in 10 children. Acta Orthop Scand 70: 275-282.
- Johnston CE (2002) Congenital pseudarthrosis of the tibia: Results of technical variations in the Charnley-Williams procedure. J Bone Joint Surg Am 84: 1799-1810.
- Johnston CE, Birch JG (2008) A tale of two tibias: A review of treatment options for congenital pseudarthrosis of the tibia. J Child Orthop 2: 133-149.
- Khan T, Joseph B (2013) Controversies in the management of congenital pseudarthrosis of the tibia and fibula. Bone Joint J 95: 1027-1034.
- Pannier S (2011) Congenital pseudarthrosis of the tibia. Orthop Traumatol Surg Res 97: 750-761.
- Pozdeev AP (2002) Pseudarthroses and defects of bones in children: Commencement address. SPb (In Russian).
- Borzunov DY, Chevardin AY, Mitrofanov AI (2016) Management of congenital pseudarthrosis of the tibia with the Ilizarov method in a paediatric population: Influence of aetiological factors. Int Orthop 40: 331-339.
- Grill F, Bollini G, Dungl P, Fixsen J, Hefti F, et al. (2000) Treatment approaches for congenital pseudarthrosis of tibia: Results of the EPOS multicenter study. European Paediatric Orthopaedic Society (EPOS) J Pediatr Orthop 9: 75-89.
- Liu YX, Mei HB, Liu K, Wu JY (2016) Correlative study between X-ray type after healing of congenital pseudarthrosis of the tibia in children and postoperative refracture. Zhonghua Wai Ke Za Zhi 54: 456-460.
- Nicolaou N, Ghassemi A, Hill RA (2013) Congenital pseudarthrosis of the tibia: The results of an evolving protocol of management. J Child Orthop 7: 269-276.
- Ofluoglu O, Davidson RS, Dormans JP (2008) Prophylactic bypass grafting and long-term bracing in the management of anterolateral bowing of the tibia and neurofibromatosis-1. J Bone Joint Surg Am 90: 2126-2134.
- Seo SG, Lee DY, Kim YS, Yoo WJ, Cho TJ, et al. (2016) Foot and ankle function at maturity after Ilizarov treatment for atrophic-type congenital pseudarthrosis of the tibia: A comprehensive outcome comparison with normal controls. J Bone Joint Surg Am 98: 490-498.
- Birke O, Schindeler A, Ramachandran M, Little DG (2010) Preliminary experience with the combined use of recombinant bone morphogenetic protein and bisphosphonates in the treatment of congenital pseudarthrosis of the tibia. J Child Orthop 4: 507-517.
- Das SP, Ganesh S, Pradhan S, Singh D, Mohanty RN (2014) Effectiveness of recombinant human bone morphogenetic protein-7 in the management of congenital pseudoarthrosis of the tibia: A randomised controlled trial. Int Orthop 38: 1987-1992.
- Friedlaender GE, Perry CR, Cole JD, Cook SD, Cierny G, et al. (2001) Osteogenic protein-1 (bone morphogenetic protein-7) in the treatment of tibial non-unions. J Bone Joint Surg Am 83: 151-158.
- Granchi D, Devescovi V, Baglio SR, Leonardi E, Donzelli O, et al. (2010) Biological basis for the use of autologous bone marrow stromal cells in the treatment of congenital pseudarthrosis of the tibia. Bone 46: 780-788.
- Lee DY, Cho TJ, Lee HR, Lee k, Moon HJ, et al. (2011) Disturbed osteoblastic differentiation of fibrous hamartoma cell from congenital pseudarthrosis of the tibia associated with neurofibromatosis type I. Clin Orthop Surg 3: 230-237.
- Lee FY, Sinicropi SM, Lee FS, Vitale MG, Roye DP Jr, et al. (2006) Treatment of congenital pseudarthrosis of the tibia with recombinant human bone morphogenetic protein-7 (rhBMP-7): A report of five cases. J Bone Joint Surg Am 88: 627-633.
- Masquelet AC, Begue T (2010) The concept of induced membrane for reconstruction of long bone defects. Orthop Clin North Am 41: 27-37.
- Pollon T, Gauzy JS, Pham T, Lemoine CT, Accadbled F (2017) Salvage of congenital pseudarthrosis of the tibia by the induced membrane technique followed by a Motorised Lengthening Nail. Orthop Traumatol Surg Res 104: 147-153.
- Richards BS, Oetgen ME, Johnston CE (2010) The use of rhBMP-2 for the treatment of congenital pseudarthrosis of the tibia: A case series. J Bone Joint Surg Am 92: 177-185.
- Soria-Sánchez CR, López-Durán A, Isunza-Ramirez A (2015) Utility of morphogenetic protein for the treatment of congenital pseudoarthrosis of the tibia. Acta Ortop Mex 29: 182-185.
- Wang W, Nyman JS, Ono K, Stevenson DA, Yang X, et al. (2011) Mice lacking Nf1 in osteochondroprogenitor cells display skeletal dysplasia similar to patients with neurofibromatosis type I. Hum Mol Genet 20: 3910-3924.
- Sakamoto A, Yoshida T, Yamamoto H, Oda Y, Tsuneyoshi M, et al. (2007) Congenital pseudarthrosis of the tibia: Analysis of the histology and the NF1 gene. J Orthop Sci 12: 361-365.
- Van Royen K, Brems H, Legius E, Lammens J, Laumen A (2016) Prevalence of neurofibromatosis type 1 in congenital pseudarthrosis of the tibia. Eur J Pediatr 175: 1193-1198.
- Kuorilehto T, Kinnunen P, Nissinen M, Alanne M, Leskelä HV, et al. (2006) Vasculopathy in two cases of NF1-related congenital pseudarthrosis. Pathol Res Pract 202: 687-690.
- Hermanns-Sachweh B, Senderek J, Alfer J, Klosterhalfen B, Büttner R, et al. (2005) Vascular changes in the periosteum of congenital pseudarthrosis of the tibia. Pathol Res Pract 201: 305-312.
- Shu-Qiang L, Yang F, Zhang X, Wang P (2008) Influence of matrix metalloproteinase on osteogenesis in the tibial periosteum of congenital pseudarthrosis. Journal of Clinical Rehabilitative Tissue Engineering Research pp: 213-216.
- Thabet AM, Paley D, Kocaoglu M, Eralp L, Herzenberg JE, et al. (2008) Periosteal grafting for congenital pseudarthrosis of the tibia: A preliminary report. Clin Orthop Relat Res 466: 2981–2994.
- Trigui M, De Billy B, Metaizeau JP, Clavert JM (2010) Treatment of congenital pseudarthrosis of the fibula by periosteal flap. J Pediatr Orthop B 19: 473-478.
- Cho TJ, Seo JB, Lee HR, Yoo WJ, Chung CY, et al. (2008) Biologic characteristics of fibrous hamartoma from congenital pseudarthrosis of the tibia associated with neurofibromatosis type 1. J Bone Joint Surg Am 90: 2735-2744.
- Engelke K, Libanati C, Fuerst T, Zysset P, Genant HK (2013) Advanced CT based in vivo methods for the assessment of bone density, structure, and strength. Curr Osteoporos Rep 11: 246-255.
- Gee CS, Nguyen JT, Marquez CJ, Heunis J, Lai A, et al. (2015) Validation of bone marrow fat quantification in the presence of trabecular bone using MRI. J Magn Reson Imaging 42: 539-544.
- Geusens P, Chapurlat R, Schett G (2014) High-resolution in vivo imaging of bone and joints: A window to microarchitecture. Nat Rev Rheumatol 10: 304-313.
- Griffith JF, Genant HK (2011) New imaging modalities in bone. Curr Rheumatol Rep 13: 241-250.
- Hiasa K, Abe Y, Okazaki Y, Nogami K, Mizumachi W, et al. (2011) Preoperative computed tomography-derived bone densities in hounsfield units at implant sites acquired primary stability. ISRN Dent p: 678729.
- Issever AS, Link TM, Kentenich M (2010) Assessment of trabecular bone structure using MDCT: Comparison of 64- and 320-slice CT using HR-pQCT as the reference standard. Eur Radiol 20: 458-468.
- Rubin GD (2014) Computed tomography: Revolutionizing the practice of medicine for 40 years. Radiology 273: 45-74.
- Tremoleda JL, Khalil M, Gompels LL, Wylezinska-Arridge M, Vincent T, et al. (2011) Imaging technologies for preclinical models of bone and joint disorders. EJNMMI Res 1: 11.
- Mahnken AH, Staatz G, Hermanns B, Gunther RW, Weber M (2001) Congenital pseudarthrosis of the tibia in pediatric patients: MR imaging. AJR Am J Roentgenol 177: 1025-1029.
- Crawford AH (1986) Neurofibromatosis in children. Acta Orthop Scand Suppl 218: 1-60.
- Gaydyshev IP (2012) AtteStat software for data analysis p: 505. Available at: /https://biostatistics.rf /files/13.pdf (access:09.10.2016) (in Russian).
- Sakamoto A, Oda Y, Iwamoto Y, Tsuneyoshi M (2007) Frequent immune-expression of TGF-beta1, FGF-2 and BMP-2 in fibroblast-like cells in osteofibrous dysplasia. Oncol Rep 17: 531-535.
- Blauth M, Harms D, Schmidt D, Blauth W (1984) Light- and electron-microscopic studies in congenital pseudarthrosis. Arch Orthop Trauma Surg 103: 269-277.
- Briner J, Yunis E (1973) Ultrastructure of congenital pseudarthrosis of the tibia. Arch Pathol 95: 97-99.
Open Access Journals
- Aquaculture & Veterinary Science
- Chemistry & Chemical Sciences
- Clinical Sciences
- Engineering
- General Science
- Genetics & Molecular Biology
- Health Care & Nursing
- Immunology & Microbiology
- Materials Science
- Mathematics & Physics
- Medical Sciences
- Neurology & Psychiatry
- Oncology & Cancer Science
- Pharmaceutical Sciences