Early Predictors of Permanent Pacemaker Implantation in Sutureless Aortic Valve Replacement with Perceval Bioprosthesis: A Conduction Disorders Analysis
Belluschi Igor*, Moriggia Stefano, Calabrese Mariachiara, Schiavi Davide and Alfieri Ottavio
Department of Cardiac Surgery, San Raffaele University Hospital, Milan, Italy
- *Corresponding Author:
- Belluschi Igor
Department of Cardiac Surgery
San Raffaele University Hospital
Via Olgettina 60, Milan, 20132, Italy
Tel: +39-02-2643-5315
E-mail: igor.belluschi@gmail.com
Received Date: December 05, 2016; Accepted Date: December 26, 2016; Published Date: December 30, 2016
Citation: Igor B, Stefano M, Mariachiara C, et al. (2016) Early Predictors of Permanent Pacemaker Implantation in Sutureless Aortic Valve Replacement with Perceval Bioprosthesis: A Conduction Disorders Analysis. J Heart Health Cir 1:1.
Copyright: © 2016 Igor B, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
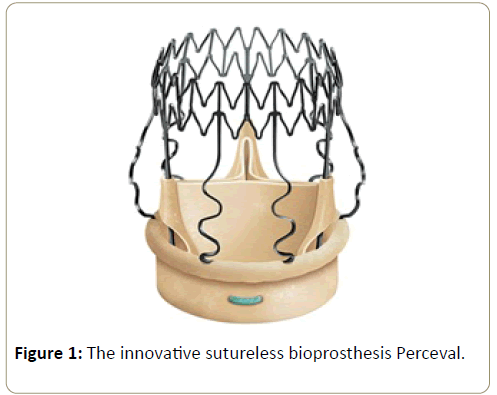
Context: The innovative Perceval bioprosthesis (Sorin Group S.p.A., Saluggia, Italy) is a surgical sutureless selfexpanding valve without a sewing ring. It has recently been introduced as an alternative to conventional surgery to minimize the operative risk in elderly patients. Advantages consist of both shortening the cardiopulmonary bypass time and enhancing the minimally invasive approach. Objective: Our study has the purpose to analyze the postoperative conduction disorders and identify the associated risk factors in patients undergoing a sutureless aortic valve replacement with the Perceval bioprosthesis. Methods: This is an observational study including 56 patients who underwent a sutureless aortic valve replacement. The conduction disorders were identified by reviewing the patients' electrocardiograms at baseline, postoperatively, before hospital discharge and at followup. Results: At baseline, five patients (8.9%) presented with pre-operative conduction disorders: two patients (3.6%) had left bundle branch block, one had right (1.8%), one right and left anterior hemiblock, while another showed a Mobitz 1 second-degree atrio-ventricular block. No one had a pre-existing permanent pacemaker. Six patients (10.7%) needed a pacemaker implantation: one for junctional rhythm with an underling atrial fibrillation, one for second-degree and four for third-degree atrioventricular block respectively. Among the 6 patients who implanted a pacemaker, four patients had preoperative conduction disorders (p<0.001) and one patient had anatomical risk factors (small aortic annulus and an offlabel concomitant mitral valve replacement). Conclusions: The presence of preoperative conduction disorders is a statistically significant risk factor for permanent pacemaker implantation following a sutureless aortic valve replacement with the Perceval bioprosthesis.
Keywords
Aortic; Valve; Sutureless; Pacemaker
Abbreviations
AV: Atrio-Ventricular
AVR: Aortic Valve Replacement
LAHB: Left Anterior Hemiblock
LBBB: Left Bundle Branch Block
LPHB: Left Posterior Hemiblock
LVOT: Left Ventricle Outflow Tract
PM: Pacemaker
PPM: Permanent Pacemaker
RBBB: Right Bundle Branch Block
SU-AVR: Sutureless Aortic Valve Replacement
TAVI: Transcatheter Aortic Valve Implantation
THV: Transcatheter Heart Valves
Introduction
Sutureless aortic valve replacement (SU-AVR) with the Perceval bioprosthesis (Figure 1) has been developed as an alternative to conventional surgery to minimize the operative risk in elderly patients, shortening the cardiopulmonary bypass time and enhancing the minimally invasive approach [1]. During the deployment of this sutureless prosthesis, the inflation at 4 atm of a ballon catheter-mounted is recommended. As for the transcatheter heart valves (THV), the implantation procedure could lead to postoperative conduction disorders. The aim of our study is to analyze the postoperative conduction disorders and identify the associated risk factors in patients undergoing SU-AVR with the Perceval bioprosthesis.
Methodology
In this observational study, 56 patients with severe aortic stenosis who underwent the implantation of the Perceval sutureless bioprosthesis at the San Raffaele University Hospital (Milan, Italy) from January 2014 to November 2016 were analyzed. The conduction disorders were identified by reviewing the patients' electrocardiograms at baseline, postoperatively, before hospital discharge and at follow-up. All tracings were analyzed by an independent investigator and an expert cardiac surgeon to record the presence of first-, secondor third-degree AV block, right bundle branch block (RBBB), left bundle branch block (LBBB), left anterior hemiblock (LAHB), left posterior hemiblock (LPHB) and arrhythmias. An experienced cardiologist gave indications whether to implant a permanent pacemaker after surgery. In our center, we wait at least 7-10 days for PM implantation. However, the decision relied on several factors and it is a well-known fact that it varies among centers, depending on the different aggressive/ early treatment approach in high risk patients with atrioventricular (AV) blocks (Figure 1).
Statistics
For the data analisys the IBM SPSS Statistic Version 22 software was used (Armonk, NY, USA). Continuous variables are reported as mean ± SD or in median and interquartile range [Q1-Q3] considering the normality of the distribution, while categorical variables are expressed by frequency (%). For continuous variables, the normality of distribution was assessed with the Kolmogorov-Smirnov test. Differences between groups are calculated using Student's T test or Mann-Whitney's U test for normal and skewed variables respectively, while Fisher’s exact test was used for categorical variables. A pvalue <0, 05 was considered to indicate statistical significance.
Results
All patients (n = 56) who underwent a SU-AVR with the Perceval bioprosthesis were included. Preoperative characteristics are shown in Table 1. The mean ± SD age of the patients was 76.9 ± 4.8 y.o., while the median Logistic EuroSCORE I was 7.7% [5.9-9.5%] and STS mortality score was 2.8% [1.9-3.7%]. At baseline, five patients (8.9%) presented with pre-operative conduction disorders: two patients (3, 6%) had LBBB, one had RBBB (1.8%), one RBBB+LAHB, while another showed a Mobitz 1 second-degree atrio-ventricular block. All the patients showed a preoperative sinus rhythm, except 3 cases of chronic atrial fibrillation. No one had a preexisting Permanent PaceMaker (PPM).
Table 1: Preoperative patients characteristics (COPD=Chronic Obstructive Pulmonary Disease, NYHA=New York Heart Association, STS=Society of Thoracic Surgeon).
| Study population | n = 56 |
|---|---|
| Age (years) | 76.9 ± 4.8 |
| Male pts | 24 (42.9%) |
| Logistic EuroSCORE I | 7.7% [5.9-9.5%] |
| STS mortality score | 2.8% [1.9-3.7%] |
| BMI | 27.7 ± 4.7 |
| Diabetes | 13 (23.2%) |
| COPD | 13 (23.2%) |
| NYHA III-IV | 16 (28.7%) |
One patient with permanent AF received a concomitant radiofrequency ablation. Six patients (10.7%) needed a PPM implantation: one for junctional rhythm with an underling atrial fibrillation, one for second-degree and four for thirddegree AV block respectively. Among the 6 patients who implanted a PPM, four patients had preoperative conduction disorders (type 1 II AV block, LBBB, RBBB and RBBB+LAHB respectively; p<0.001) and one patient had anatomical risk factors (small aortic annulus and an off-label concomitant mitral valve replacement).
The PM implantation procedure was performed 7-40 days after surgery (median: 18 days). Of the 6 patients requiring a PPM implantation, an arithmologic follow-up was available in 4 patients (66.7%), while one subject with PPM died after 9 months from surgery for senile marasmus.
The median follow-up duration was 5.9 months (2.9-13.7). Of the 4 patients, 3 (75%) were pacemaker dependent and 1 (25%) was nonpacemaker dependent (Table 2).
Table 2: PPM rate in SU-AVRs with Perceval in literature.
| Author | Center | No. of pts | PPM (%) |
|---|---|---|---|
| Flameng et al. [3] | Leuven, Belgium | 32 | 3.10% |
| Folliguet et al. [4] | Paris, France - Hannover, Germany | 208 | 7.70% |
| Mazine et al. [5] | Canadian multicenter study | 215 | 17% |
| Van Boxtel et al. [6] | Eindhoven, Germany | 30 | 13.30% |
| Konig et al. [7] | Jena, Germany | 14 | 28.50% |
| Vogt et al. [8] | Nuremberg - Münster, Germany | 258 | 10.50% |
| Shresta et al. [1] | European multicenter study | 731 | 7.40% |
| Belluschi et al. 2016 | Milan, Italy | 56 | 10.70% |
Discussion
The identification of risk factors associated with a PPM implantation after aortic valve surgery is still an open issue, even more in the setting of sutureless valves [2].
The exact mechanism of atrioventricular conduction disorders in SU-AVRs with Perceval remains to be clearly elucidated. Some hypothesis include: the decalcification process, the large annular sealing coil of the inflow ring, the balloon inflation at 4 atm (3040 mmHg) and the high profile of the nitinol stent. The patients who mostly benefit by using a sutureless procedure are at intermediate/high surgical risk, with higher rates of surgical complications. However, our idea is that the surgeon’s sutureless experience plays a pivotal role. New recommendations for implant by LivaNova, to avoid any interference with the conduction system, consist of both the undersizing approach and the evaluation of the guiding sutures depth. The four Perceval dedicated sizers (size S for annuli 19-21 mm; M for 21-23 mm; L for 23-25 mm; XL for 25-27 mm; Figure 2) are used to assess the corresponding prosthesis size: in case of doubt between two sizes the best choice is the smaller size. This precaution could reduce the development of paravalvular leaks, intra-aortic regurgitation, high gradients and postoperative PM need. Furthermore, the surgical procedure required the application of three 4-0 Prolene guiding sutures. New recommendations suggest their insertion at 1-2 mm below the nadir of each aortic cusps into the LVOT (previous manufacturer's guidelines reported 3-4 mm). In addition, a normal bite of the stitches has to be considered to reduce a possible trauma of the His bundle.
It seems to be interesting to investigate the percentage of patients who are still pacemaker dependent at follow-up and whether rhythm disorders recover over time. In our population, 75% of the PM receivers were pacemaker dependent at the available arithmologic follow-up.
The majority of PM was implanted after hospital discharge: the median interval of the arrhythmological procedure from surgery was 18 days (5 subjects received a PM>10 days from operation), while the median postoperative hospital stay was 6 days.
Our results are quite similar to those provided by other groups using Perceval, even if there is a great variability. The belgian group of Flameng first reported in 2011 a very low PPM rate of 3.3% [3], while the beginning experience of 208 patients treated with Perceval in France and Germany showed a rate of 7.7% [4]. In the canadian multicenter study the rate was 17% [5]. In the serie of Van Boxtel, 4 patients needed a PPM implantation (13.3%) [6], while the group of Konig reported a rate of 28.5%, the highest described about Perceval, but in a very small serie, therefore maybe affected by the learning curve [7]. The group directed by Santarpino in Germany published a percentage of 10.5% [8], while the largest serie belonged to the European multicenter study (Pilot, Pivotal, CAVALIER trials) of 731 patients with a rate of 7.4% [1].
These results are comparable to the conventional AVRs with sutured bioprosthesis. As reported by Huynh et al. [9] and Elahi et al. [10] the PPM implantation rates varies from 8.7-9.1% to 8.3-18% for stented and stentless AVRs respectively. Small aortic annulus, pre-operative rhythm disorders (OR=12.5) and concomitant mitral valve replacement (OR=11.5) were identified as risk factors.
The need of PPM implantation for other sutureless devices seems to be lower than Perceval. Borger et al. [11] showed a rate of 5% in their AVRs with the rapid deployment system Edwards Intuity (7/141). A similar percentage was obtained in the serie of Eichstaedt et al. [12] in which 120 patients were treated with the 3f Enable valve: among them, only 8 patients needed a PM (6.7%). In a meta-analysis published in 2011 by Bates et al. [13] the mean PPM implantation rate following a TAVI procedure was 14.2%, even if it appeared higher in case of Medtronic CoreValve (20.8%), while the Edwards Sapien device showed a percentage of 5.4%.
In their serie of 258 SU-AVRs with Perceval, Vogt et al. identified age and preoperative RBBB as independent predictors of PPM implantation [8]. In our study, the presence of preoperative conduction disorders (II-degree AV block, LBBB, RBBB and RBBB+LAHB) was found to be a risk factor for PPM implantation [overall n= 5 (8.9%), PPM vs no-PPM group: 4 vs 1 (66.7% vs 2%); p<0,001].
The main limit of this study was the small number of patients. In addition, our population includes the first 56 patients who underwent a SU-AVR with the Perceval bioprosthesis at our center; therefore these results could be affected by the surgeon’s learning curve. So, further investigations and randomized clinical trials are mandatory to identify other risk factors and the impact of the SU-AVR implantation technique on the rate of PPM implantation.
In conclusion, the presence of preoperative conduction disorders is a statistically significant risk factor for PPM implantation following a SU-AVR with the Perceval bioprosthesis. Therefore, despite Perceval’s optimal hemodynamic results, an accurate analysis of the preoperative rhythm has to be considered.
A written consent was obtained from each patient after full explanation of the purpose and nature of the procedures used.
Disclosure
Dr. Stefano Moriggia has a financial relationship with Sorin Group S.p.A. as proctor for Perceval.
References
- Shrestha M, Fischlein T, Meuris B, Flameng W, Carrel T, et al. (2015) European multicentre experience with the sutureless Perceval valve: clinical and haemodynamic outcomes up to 5 years in over 700 patientsdagger. Eur J Cardiothorac Surg 49: 234-241.
- Matthews IG, Fazai IA, Bates MG, Turley AJ (2011) In patients undergoing aortic valve replacement, what factors predict the requirement for permanent pacemaker implantation? Interact Cardiovasc Thorac Surg 12: 475-479.
- Flameng W, Herregods MC, Hermans H, Van der Mieren G, Vercalsteren M, et al. (2011) Effect of sutureless implantation of the Perceval S aortic valve bioprosthesis on intraoperative and early postoperative outcomes. J Thorac Cardiovasc Surg 142(6):1453-1457.
- Folliguet TA, Laborde F, Zannis K, Gorhayeb G, Haverich A, et al. (2012) Sutureless perceval aortic valve replacement: results of two European centers. Ann Thorac Surg 93: 1483-1488.
- Mazine A, Teoh K, Bouhout I, Bhatnagar G, Pelletier M, et al. (2015) Sutureless aortic valve replacement: a Canadian multicentre study. Can J Cardiol 31: 63-68.
- Van Boxtel AG, Houthuizen P, Hamad MA, Sjatskig J, Tan E, et al. (2014) Postoperative conduction disorders after implantation of the self-expandable sutureless percevals bioprosthesis. J Heart Valve Dis 23: 319-324.
- Konig KC, Wahlers T, Scherner M, Wipperman J (2014) Sutureless perceval aortic valve in comparison with the stented Carpentier-Edwards perimount aortic valve. J Heart Valve Dis 23: 253-258.
- Vogt F, Pfeiffer S, Dell’Aquila AM, Fischlein T, Santarpino G (2016) Sutureless aortic valve replacement with Perceval bioprosthesis: are there predicting factors for postoperative pacemaker implantation. Interact Cardiovasc Thorac Surg 22: 253-258.
- Huynh H, Dalloul G, Ghanbari H, Burke P, David M, et al. (2009) Permanent pacemaker implantation following aortic valve replacement: current prevalence and clinical predictors. Pacing Clin Electrophysiol 32: 1520-1525.
- Elahi M, Usmaan K (2006) The bioprosthesis type and size influence the postoperative incidence of permanent pacemaker implantation in patients undergoing aortic valve surgery. J Interv Card Electrophysiol 15: 113-118.
- Borger MA, Dohmen P, Misfeld M, Mohr FW (2013) Minimal invasive implantation of an EDWARDS INTUITY rapid deployment aortic valve. Multimed Man Cardiothorac Surg.
- Eichstaedt HC, Easo J, Harle T, Dapunt OE (2014) Early single-center experience in sutureless aortic valve implantation in 120 patients. J Thorac Cardiovasc Surg 147: 370-375.
- Bates MG, Matthews IG, Fazai IA, Turley AJ (2011) Postoperative permanent pacemaker implantation in patients undergoing trans-catheter aortic valve implantation: what is the incidence and are there any predicting factors. Interact Cardiovasc Thorac Surg 12: 243-253.
Open Access Journals
- Aquaculture & Veterinary Science
- Chemistry & Chemical Sciences
- Clinical Sciences
- Engineering
- General Science
- Genetics & Molecular Biology
- Health Care & Nursing
- Immunology & Microbiology
- Materials Science
- Mathematics & Physics
- Medical Sciences
- Neurology & Psychiatry
- Oncology & Cancer Science
- Pharmaceutical Sciences