Sinonasal Extranodal Sinus Histocytosis Mimicking Malignant Sarcomas
Department of Pathology, UC Irvine Medical Center, UC Irvine School of Medicine, USA
- *Corresponding Author:
- Ifegwu Ibe
Department of Pathology, UC Irvine Medical Center
UC Irvine School of Medicine, USA
Tel: 001-714-456-7890
E-mail: iibe@uci.edu
Received date: December 26, 2017; Accepted date: January 15, 2018; Published date: January 22, 2018
Citation: Ibe I, Nowroozizadeh B, Zhao XS, Goreal W, Bhandarkar N (2017) Sinonasal Extranodal Sinus Histocytosis Mimicking Malignant Sarcomas. J Med Oncol Vol.1 No.1:3
Copyright: ©2017 Ibe I, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution and reproduction in any medium, provided the original author and source are credited
Abstract
Sinus histocytosis with massive lymphadenopathy, aka Rosai-Dorfman disease (RDD) is a rare, non-hereditary, histiocytic proliferative disorder, usually involving lymph nodes but occasionally occurring in extranodal sites. Extranodal involvement can be seen prior to,concurrently with, or post-nodal disease. We report two cases of extranodal sinonasal Rosai-Dorfman disease with initial mass morphology resembling high-grade sarcomas, on intraoperative consultation. Histopathology revealed large atypical spindly histiocytes with scattered emperipolesis. Immunohistochemistry was useful to determine the nature of the masses as the large atypical cells were positive for S100 and histiocytic markers CD68 and CD163. Recognition of sinonasal presentation of extranodal Rosai-Dorfman disease and its ability to histologically mimic other spindle cell neoplasms ensures accurate diagnosis for treatment.
Keywords
Histocytosis; Sinonasal; Myofibroblastic; Neuroblastoma; Paranasal
Introduction
Sinus histocytosis with massive lymphadenopathy, aka Rosai- Dorfman disease (RDD) is a rare, non-hereditary, histiocytic proliferative disorder, usually involving lymph nodes but occasionally occurring in extranodal sites including skin, soft tissue, skeletal system, central nervous system and head and neck areas [1,2]. Involvement of paranasal sinuses is very rare. [2]. We are reporting two rare cases of sinonasal extranodal sinus histocytosis with initial mass morphology resembling malignant sarcomas. Immunohistochemistry was useful to determine the nature of both masses. This rare sinonasal presentation of extranodal RDD mimicking malignant neoplasms can create diagnostic and therapeutic challenges.
Case Report
The first case, a 61 year old male with chief complaint of difficulty breathing presented with bilateral polypoid sinonasal masses that elevated the nasal floor, and involved the anterior nasal septum, lateral wall and paranasal sinuses with severe nasal obstruction. Due to location of the lesion and patient’s symptoms, the mass was endoscopically excised. During intraoperative consultation, the mass morphologically presented as a pleomorphic spindle cell neoplasm with scattered large atypical spindle cells, resembling a high-grade sarcoma (Figure 1).
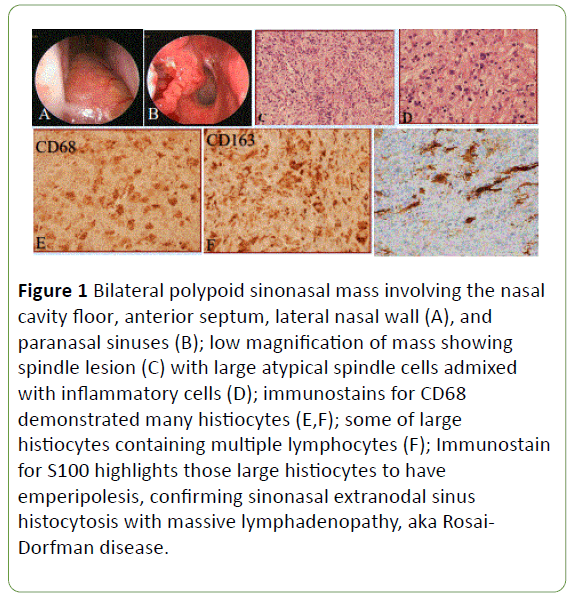
Figure 1: Bilateral polypoid sinonasal mass involving the nasal cavity floor, anterior septum, lateral nasal wall (A), and paranasal sinuses (B); low magnification of mass showing spindle lesion (C) with large atypical spindle cells admixed with inflammatory cells (D); immunostains for CD68 demonstrated many histiocytes (E,F); some of large histiocytes containing multiple lymphocytes (F); Immunostain for S100 highlights those large histiocytes to have emperipolesis, confirming sinonasal extranodal sinus histocytosis with massive lymphadenopathy, aka Rosai- Dorfman disease.
The second case, a 46 year old male, presented with recurrent bilateral maxillary chronic sinusitis with mass formation, clinically suspicious for malignant lymphoma. The patient has subsequently been treated by surgical resection of the disease four times. He has complaints of nasal congestion and decreased nasal ventilation. Excisional biopsies were performed. Histopathology of his sinonasal masses showed large irregular spindly histocytes with abundant granular and vacuolated cytoplasm. The morphology of both cases revealed large atypical spindly histiocytes, resembling fibrohistiocytic or myofibroblastic proliferative neoplasms (Figure 2). Immunohistochemical studies were performed on both cases which demonstrated that the large atypical cells were positive for S100 and histiocytic markers CD68 and CD163, with scattered emperipolesis noted. No expression for sarcoma or lymphoma markers, such as CD34, CD117, PAX5, MUM-1 and vimentin were identified. Both cases were confirmed as extranodal sinus RDD.
Figure 2:Excisional biopsy showing sinonasal mucosa with chronic inflammation and lymphocytes (A); closer view showing irregular histiocytic proliferation (B) with granular and vacuolated cytoplasm (C). Immunostains show lesional cells were positive for S100 (D) and CD68, consistent with sinonasal extranodal sinus Rosai-Dorfman disease.
Discussion
Rosai-Dorfman disease is a rare, self-limiting disease classified within the spectrum of histiocytic disorders. It is more common in children and young adults and usually presents with massive painless cervical lymphadenopathy. Extranodal involvement is identified in more than 25% of the patients, and the most commonly involved organs are the skin, paranasal sinuses, orbit, bone, salivary gland, and central nervous system [3-6]. Extranodal involvement can be seen prior to, concurrently with, or after nodal disease [7]. Diagnosis is more challenging when the patient presents with only extranodal involvement as seen in our cases.
Histopathology of Rosai-Dorfman disease shows proliferated and distended lymphatic sinuses with infiltration of lymphocytes, plasma cells with Russell bodies and large histiocyte-like cells with vesicular nucleus and large cytoplasm, and the structure of the lymphatic sinus is partially or completely effaced as a result. The most significant histopathological finding of the disease is the detection of phagocytized intact lymphocytes, plasma cells and erythrocytes within the cytoplasm of the large histiocyte-like cells; this has been designated as emperipolesis. Emperipolesis is seen less frequently in extranodal disease which adds to the difficulty in diagnosis [3].
In cases of paranasal sinus involvement, nasopharyngeal carcinoma and olfactory neuroblastoma should be considered as the main differential diagnosis. Histiocytic proliferative diseases such as Langerhans cell histiocytosis are among the differential diagnoses. In addition, Wegener’s granuloma, Hodgkin’s lymphoma, tuberculosis, sarcoidosis, inflammatory pseudotumor, reactive sinus hyperplasia and plasma cell granuloma should be considered [3,4,7].
In both of our cases, histopathologic evaluation showed large irregular spindly histocytes with abundant granular and vacuolated cytoplasm. The morphology of both cases revealed large atypical spindly histiocytes, resembling fibrohistiocytic or myofibroblastic proliferative neoplasms with scattered emperipolesis. Making a diagnosis based only on the histologic features is difficult especially during intraoperative consultation. Immunohistochemically, the large atypical spindle cells revealed staining for S100 protein and histiocytic markers CD68 and CD163 but were negative for sarcoma or lymphoma markers, such as CD34, CD117, PAX5, MUM-1 and vimentin. The above histopathological and immunohistochemical findings confirmed the diagnosis of extranodal sinus Rosai-Dorfman disease. Extranodal RDD should be considered in paranasal and nasal cavity masses, although presentation at these sites is very rare.
Commonly, RDD has a benign course and undergoes complete spontaneous resolution. However, some cases with widespread extranodal involvement can affect vital organs and cause functional disorder, thus resulting in surgical intervention. Other treatment regimens include chemotherapy, radiation, interferon, acyclovir, monoclonal antibody treatment, and steroids. [2,5,7,8] In our cases, the masses entirely filled the paranasal sinuses and caused difficulty in breathing, thus they were excised surgically.
Conclusion
In summary, Rosai-Dorfman disease (RDD) is a rare histiocytic disorder with propensity to cause massive painless cervical lymphadenopathy. Extranodal involvement which is common and present in nearly half of the patients with RDD, can be seen prior to, concurrently with, or after nodal disease. Extranodal RDD can be morphologically confused with spindle cell neoplasms. This can create a major diagnostic challenge, especially during intraoperative consultation. It is critical to recognize this rare mimicking pitfall so as to provide accurate diagnosis for treatment. Identification of atypical histiocytes showing emperipolesis and S100 positivity helps confirm the diagnosis.
References
- Chang YC, Tsai MH, Chen CL, Tsai CH, Lee AY (2003) Nasal Rosai-Dorfman disease with intracranial involvement: a case report. Am J Otolaryngol 24: 183-186.
- Mohanty S, Gopinath M (2014) Rosai Dorfman disease mimicking as paranasal sinus malignancy. J Case Rep 4: 236-239.
- Akyigit A, Akyol H, Sakallioglu O, Polat C, Keles E, et al. (2015) Rosai-Dorfman disease originating from nasal septal mucosa. Case Rep Otolaryngol 232898.
- Dodson KM, Powers CN, Reiter ER (2003) Rosai Dorfman disease presenting as synchronous nasal and intracranial masses. Am J Otolaryngol 24: 426-430.
- Ashish G, Chandrashekharan R, Parmar H (2016) Rare case of Rosai Dorfman disease involving paranasal sinuses in paediatric patient: A case report. Egypt J Ear Nose Throat Allied Sci 17: 43-46.
- Gupta L, Batra K, Motwani G (2005) A rare case of Rosai-Dorfman disease of the paranasal sinuses. Indian J Otolaryngol Head Neck Surg 57: 352-354.
- Khan AA, Siraj F, Rai D, Aggarwal S (2011) Rosai-Dorfman disease of the paranasal sinuses and orbit. Hematol Oncol Stem Cell Ther 4: 94-96.
- Carbone A, Passannante A, Gloghini A, Devaney KO, Rinaldo A, et al. (1999) Review of sinus histiocytosis with massive lymphadenopathy (Rosai-Dorfman disease) of head and neck. Ann Otol Rhinol Laryngol 108: 1095-1104.
Open Access Journals
- Aquaculture & Veterinary Science
- Chemistry & Chemical Sciences
- Clinical Sciences
- Engineering
- General Science
- Genetics & Molecular Biology
- Health Care & Nursing
- Immunology & Microbiology
- Materials Science
- Mathematics & Physics
- Medical Sciences
- Neurology & Psychiatry
- Oncology & Cancer Science
- Pharmaceutical Sciences