Elastofibroma Dorsi of the Lateral Chest Wall Deep to Serratus Anterior and Latissimus Dorsi Muscles: A Case Report
1Department of Orthopaedic Surgery and Traumatology, Saint Georges University Medical Center, Balamand University, Achrafieh, Beirut, Lebanon
2Saint Georges University Medical Center, Balamand University, Achrafieh, Beirut, Lebanon
- *Corresponding Author:
- Joseph Maalouly
Department of Orthopaedic Surgery and Traumatology
Saint Georges University Medical Center, Balamand University
P.O.Box 166378, Achrafieh, Beirut, 1100 2807, Lebanon
Tel: 009613331779
E-mail: josephmaalouly2@gmail.com
Received date: July 25, 2018; Accepted date: August 08, 2018; Published date: August 14, 2018
Citation: Maalouly J, Aouad D, Nour HA, Ayoubi R, Wehbi J, et al. (2018) Elastofibroma Dorsi of the Lateral Chest Wall Deep to Serratus Anterior and Latissimus Dorsi Muscles: A Case Report. J Orthop Disord Vol.1: No.1: 3.
Abstract
Elastofibroma dorsi (EFD) is a rare benign soft tissue tumor composed of collagen and elastic fibers, often asymptomatic and non-painful mobile mass in the back. It can also present as a painful swelled mass causing discomfort and snapping of the scapula. Our case is a 49- year-old female patient with a typical presentation of non-painful 10 cm mass in the subscapular area, with no other symptoms, discovered by incident. Imaging and biopsy confirmed the diagnosis of EFD; the tumor was excised through the Posterolateral Thoracotomy Approach with no significant complications. Currently, there are no specific guidelines for excision of EFD, yet it is advised to excise surgically whenever the mass exceeds 10 cm. It is also recommended to do the latter for symptomatic relief or for esthetic reasons. Close follow up must be done for a possible hematoma formation or recurrence of the tumor.
Keywords
Elastofibroma dorsi; Benign tumor
Introduction
Elastofibroma dorsi (ED) is a type of rare, slowly-progressing benign tumor of the lower subscapular region, firstly described by Jarvi and Saxen, 1961 [1]. It is usually located deep to serratus anterior, often attached to the periosteum of the ribs in the inferior scapular angle [2]. The tumor usually presents as a non-encapsulated, poorly defined, solitary mass composed of fragmented and enlarged elastic fibers embedded in collagenous matrix surrounded by streaks of fatty acids [1,3-5]. Although the majority of patients are asymptomatic on presentation, complaining uniquely of the presence of a mass [3], it can also be associated with a history of swelling, discomfort, snapping of the scapula and pain [1,3,5]. Elastofibroma dorsi occurs mainly in active older individuals with a mean age of 70-years-old, more common in women and believed to be due to repetitive microtrauma [3,4]. MRI is an important tool for the diagnosis of ED showing characteristic patterns and it is debatable whether a biopsy is needed to confirm the diagnosis [6]. Surgical excision is recommended for symptomatic or large tumors with complications including hematoma postop, seroma formation and recurrence.
Case Report
This is the case of a 49-year-old female who presented with a non-painful mass in the subscapular area discovered incidentally 3 months ago. The mass was described as mobile and progressively increasing in size reaching about 10 cm on physical exam. No neurologic symptoms or decrease in the range of motion were reported by the patient or on examination.
Investigation
Following these findings, further investigations were carried. An MRI of the left chest wall was first performed using 1.5 T magnet in the following planes and sequences: Axial T1, T2 FSE and T2 Fat Sat; Coronal T1 TSE; Sagittal T2 FSW.
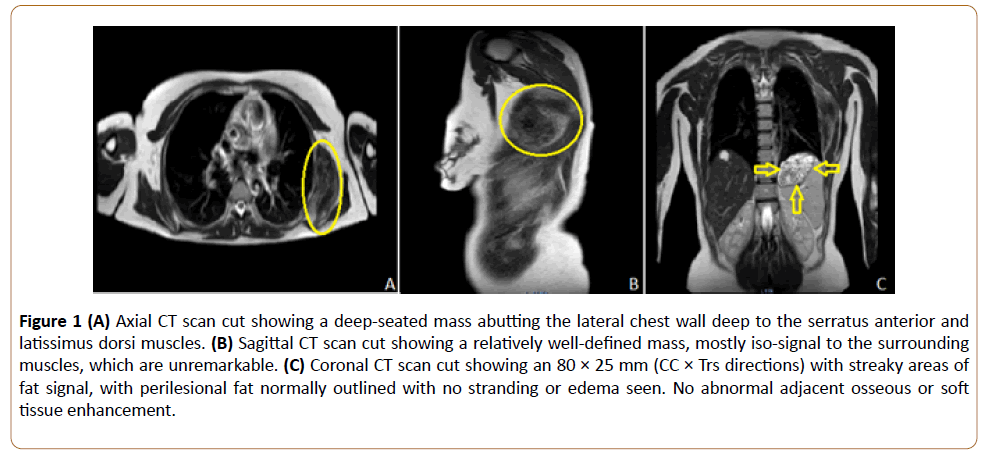
The imaging revealed the presence of a profound mass adjacent to the lateral chest wall, deep to the serratus anterior and latissimus dorsi muscles. The mass measured 80 × 66 × 25 mm (CC × Ap × Trs directions). The mass was well defined, mostly isosignal to muscles on all sequences, with streaky area of fat signal.
Following the injection of contrast, only this mass has shown faint linear enhancement, (Figure 1) showing a relatively welldefined mass, mostly isosignal to the surrounding muscles, which are unremarkable. C: Coronal CT scan cut showing an 80 × 25 mm (CC × Trs directions) with streaky areas of fat signal, with perilesional fat normally outlined with no stranding or edema seen. No abnormal adjacent osseous or soft tissue enhancement.
Figure 1: (A) Axial CT scan cut showing a deep-seated mass abutting the lateral chest wall deep to the serratus anterior and latissimus dorsi muscles. (B) Sagittal CT scan cut showing a relatively well-defined mass, mostly iso-signal to the surrounding muscles, which are unremarkable. (C) Coronal CT scan cut showing an 80 × 25 mm (CC × Trs directions) with streaky areas of fat signal, with perilesional fat normally outlined with no stranding or edema seen. No abnormal adjacent osseous or soft tissue enhancement.
Subsequently, a true cut biopsy was obtained from the mass and four filiform fragments were sent to the histology laboratory, the samples size varied from 0.5 × 0.1 to 0.2 × 0.1. Histological cut made from the sample revealed oligo-cellular soft tissue mass with collagen bundles deposit alternating with numerous acidophilic cylinders. Those cells often contained a central dense core. They stain strongly with elastic stains – Orcein. Both the histological features seen, and the imaging findings correspond to Elastofibroma.
Surgical intervention
Based on that diagnosis, the Posterolateral Thoracotomy Approach was used to excise the tumour. The patient was in lateral decubitus position, with a free draping of the arm that was placed on a padded mayo stand.
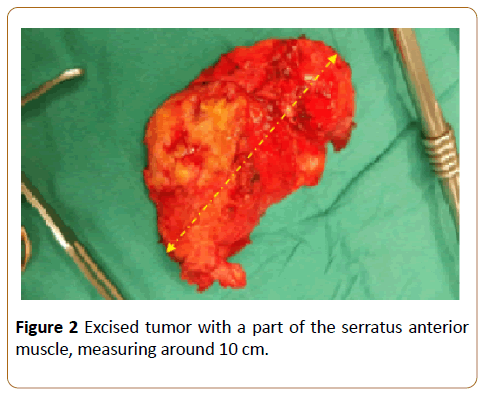
A curvilinear incision cantered was made Posterolateral; a deep dissection was performed at the Triangle of Auscultation, the interval between the Latissimus, Trapezius, and the inferior Scapular border (alternatively, the Latissimus can be split in line with its fibres depending on the location of the ribs). The underlying Serratus was then split in line with its fibres to expose the ribs. The tumour was now seen and found to be adherent to the serratus anterior fibres and embedded within its fibres. Excision of the tumour with a part of the serratus anterior muscle was performed successfully: the excised part measured about 10 cm (Figure 2).
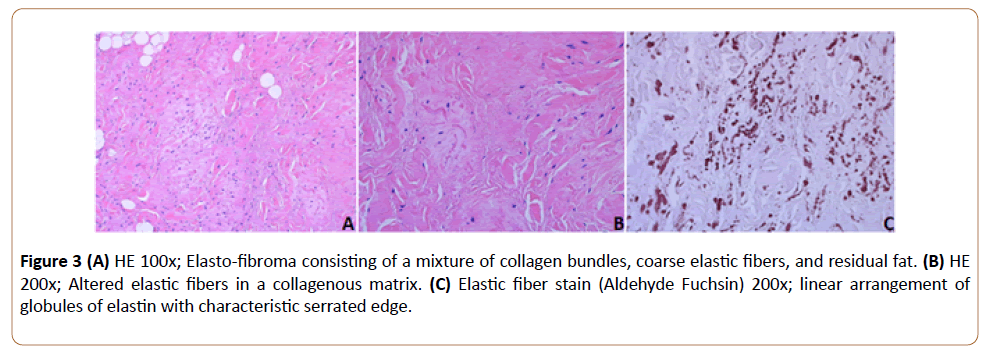
All layers at the incision were closed adequately, and compressive dressings were applied postop. After one month, the patient presented for follow up, there was no hematoma found and patient retained full range of motion. Following the excision, the tumor was sent to the pathology lab where further investigation confirmed the diagnosis. A special stain, the Elastic fibre stain Aldehyde Fuchsin was used to reveal the specific characteristic of this tumour’s fibres (Figure 3).
Figure 3: (A) HE 100x; Elasto-fibroma consisting of a mixture of collagen bundles, coarse elastic fibers, and residual fat. (B) HE 200x; Altered elastic fibers in a collagenous matrix. (C) Elastic fiber stain (Aldehyde Fuchsin) 200x; linear arrangement of globules of elastin with characteristic serrated edge.
Discussion
First described in 1961 by Jarvis and Saxen, the World Health Organization put Elastofibroma Dorsi under the category of benign fibroblast/myofibroblast tumor, according to Pradeep et al. [7]. In fact, this tumor can be erroneously diagnosed as soft tissue sarcoma [8]. EFD usually occurs in the elderly population, with a mean age of onset of 70-years, and predominantly in females rather than males [9]. As noted previously, EFD is a rare and slow growing tumor of the soft tissue usually located at the inferior subscapular region. As it is generally asymptomatic, it is found by happenstance on radiological imaging [9]. EFD was found to cause snapping of the scapula in some patient, this being considered the only major symptom affecting the course of treatment [10].
While the pathophysiology of EFD is not fully understood, a mechanical cause consisting of a friction between the scapula and the chest wall is favoured, especially due to physical activity [10]. It is suggested that the process involves collagen degeneration and elastic fibres fragmentation and hypertrophy [11]. However, family history of EFD and new cytogenetic and genetic studies suggest that chromosomal aberrations can be at the basis of this disease [9]. In the case of EFD, the use of biopsy is debatable [9]. Go et al., suggest starting with an ultrasound to diagnose EFD and thus preventing the use of biopsy and surgical approach to the tumor [12]. In fact, the patient history, symptoms and physical exam together with the findings, such as low intensity and well-defined borders with enhancement with gadolinium, [13] on ultrasound or MRI are enough to diagnose EFD. Currently, it is recommended to perform a surgical excision of the mass only in symptomatic patients or patients that desire so [10]. It is noted that the major postoperative complication is hematoma which is treated conservatively [10]. While no malignancy is noted, EFD has a high rate of recurrence if not properly excised, about 7%, where radiotherapy can be helpful to prevent this phenomenon [9].
Conclusion
In conclusion, EFD is a rare and benign soft tissue tumor of the elderly population, localized in the subscapular region. While it is mostly asymptomatic, it is advised to remove if measuring more than 10 cm, as in this case presented above. Investigations being a must, in our case, the MRI findings, true cut biopsies and post-operative histological studies of the excised mass all confirmed the diagnosis of EFD. On follow up one month later, no hematoma was noticed, and the patient had retained full range of motion. Further follow up with this patient must be done, as this tumor was found to have a significant recurrence rate.
References
- Järvi O, Saxén A, Hopsu-Havu V, Wartiovaara J, Vaissalo V (1969) Elastofibroma: A degenerative pseudotumor. Cancer 23(1): 42-63.
- Chandrasekar C, Grimer R, Carter S, Tillman R, Abudu A, et al. (2008) Elastofibroma dorsi: An uncommon benign pseudo-tumor. Sarcoma pp: 1-4.
- Nagamine N, Nohara Y, Ito E (1982) Elastofibroma in Okinawa: A clinicopathologic study of 170 cases. Cancer 50(9): 1794-1805.
- Malghem J, Baudrez V, Lecouvet F, Lebon C, Maldague B, et al. (2004) Imaging study findings in elastofibroma dorsi. Joint Bone Spine 71(6): 536-541.
- Chamberlain R, Go P, Meadows M, BE Deleon (2010) Elastofibroma dorsi: A soft tissue masquerade. Int J Shoulder Surg 4(4): 97.
- Muramatsu K, Ihara K, Hashimoto T, Seto S, Taguchi T (2007) Elastofibroma dorsi: Diagnosis and treatment. J Shoulder Elbow Surg 16(5): 591-595.
- Goyal P, Gandhi D, Gupta S, Li S, Kumar Y, et al. (2017) Elastofibroma dorsi. Proceedings, Baylor University. Medical Center 30(3): 340–342.
- Smith H, Hannay J, Thway K, Messiou C, Smith M, et al. (2016) Elastofibroma dorsi: The clunking tumour that need not cause alarm. Ann R Coll Surg Engl 98(3): 208–211.
- Sehli SA, Salah MB, Smichi I, Koubaa W, Khayat O, et al. (2015) Adventitious discovery of elastofibroma dorsi on skin biopsy 2: 1.
- Nagano S, Yokouchi M, Setoyama T, Sasaki H, Shimada H, et al. (2014) Elastofibroma dorsi: Surgical indications and complications of a rare soft tissue tumor. Mol Clin Oncol 2(3): 421–424.
- MartÃÂÂnez Hernández NJ (2011) Elastofibroma dorsi bilateral: Una muy rara presentación para una rara patologÃÂÂa. Arch Bronconeumol 47: 536–537.
- Meadows Go PH, Deleon MC, Chamberlain RS (2010) Elastofibroma dorsi: A soft tissue masquerade. Int J Shoulder Surg 4(4): 97–101.
- Razek AA, Huang BY (2011) Soft tissue tumors of the head and neck: Imaging-based review of the WHO classification. Radiographics 31: 1923-1954.
Open Access Journals
- Aquaculture & Veterinary Science
- Chemistry & Chemical Sciences
- Clinical Sciences
- Engineering
- General Science
- Genetics & Molecular Biology
- Health Care & Nursing
- Immunology & Microbiology
- Materials Science
- Mathematics & Physics
- Medical Sciences
- Neurology & Psychiatry
- Oncology & Cancer Science
- Pharmaceutical Sciences