Evaluation of Demographic, Clinical, Laboratory Findings and Treatments of Our Febrile Seizures Cases
Ozge Yilmaz*
Department of Research and Development, Bilkent University, Çankaya/Ankara, Türkiye
- *Corresponding Author:
- Ozge Yilmaz
Department of Research and Development, Bilkent University, Çankaya/Ankara, Türkiye
E-mail:turk14531920@mynet.com
Received date: August 28, 2024, Manuscript No. IPIJCR-24-19579; Editor assigned date: August 30, 2024, PreQC No. IPIJCR-24-19579 (PQ); Reviewed date: September 17, 2024, QC No. IPIJCR-24-19579; Revised date: January 08, 2025, Manuscript No. IPIJCR-24-19579 (R); Published date: January 15, 2025, DOI: 10.36648/IPIJCR.9.1.008
Citation: Yilmaz O (2025) Evaluation of Demographic, Clinical, Laboratory Findings and Treatments of Our Febrile Seizures Cases. Int J Case Rep Vol: 9 No:1
Abstract
The most common type of convulsion seen in children is Febrile Convulsions (FC). According to the American Academy of Pediatrics, FC is defined as a convulsion occurring between 6 and 60 months of age, caused by a fever due to an infection affecting the Central Nervous System (CNS) or without another identified cause (such as electrolyte imbalance, intoxication, metabolic disorder, or trauma), in children who didn't have afebrile convulsion before. The frequency of febrile convulsions can vary in different studies, ranging between 4-5%. It is estimated to be 5-10% in some regions of the world. The variation in the frequency of FC among different countries and regions is thought to be multifactorial, including local environmental factors and genetic reasons. Boys are more effected than girls. The male to female ratio is approximately 1.4:1. It has been found that children with a family history of FC have a fourfold increased risk compared to the general population. FCs are most commonly seen between 18-22 months of age. They are triggered when the axillary body temperature reaches 38.5°C and usually develop within 1-2 hours after the onset of fever. Upper Respiratory Tract Viral Infections (URTI) are seen to cause FC more frequently than other infections. In this study, we aimed to determine the sociodemographic, clinical, and laboratory characteristics of patients diagnosed with FC who presented to our clinic, for evaluating their responses to applied treatment options, and to identify risk factors for epilepsy development and FC recurrence, taking into account the importance of close monitoring and careful assessment of these patients.
Keywords
Prevalence; Traditional medicine practices; Mothers; Under-five children; Owerri
Introduction
Our study was conducted at the Pediatric Neurology Department of Trakya University Medical Faculty, Child Health and Diseases Outpatient Clinic, with patients diagnosed with FC who were followed up between January 2014 and April 2018. FC was defined as convulsions occurring between the ages of 6 months to 5 years, associated with fever of at least 38°C without CNS infection, metabolic imbalance, or a history of afebrile seizures. The convulsions lasting less than 15 minutes, not recurring within 24 hours, and without focal characteristics were classified as Simple Febrile Convulsions (SFC). Convulsions lasting longer than 15 minutes, recurring within 24 hours, or showing focal characteristics were classified as Complex Febrile Convulsions (CFC). Recurrence was defined as the reappearance of a convulsion at a different time period not associated with the same illness course. Epilepsy was diagnosed in patients who had at least two unprovoked seizures 24 hours apart. Patients' files were retrospectively reviewed, including data from the hospital's information system, laboratory tests, and radiological imaging results. The included cases were analyzed for gender, age at onset of FC, birth history, parental consanguinity, family history of FC and epilepsy, type of seizure, and clinical and laboratory findings [1-5].
Materials and Methods
The data regarding the form, duration, fever focus, body temperature during the seizure, frequency of FK seizures, and the effectiveness of the antiepileptics used by the patients, laboratory results, lumbar puncture, EEG and MR results were evaluated. Laboratory results including C-reactive protein and LP puncture results were evaluated alongside reference values from trakya University Faculty of Medicine's laboratory, hemogram results were evaluated together with pediatric age group normal reference values. Patients' data were transferred to the "Patient Follow-up Form."
Statistical analysis
For the evaluation of the research data, "Statistical Package for the Social Sciences" version 19.0 was used. Categorical variables in the study were shown as number (n) and percentage (%), while numerical data were presented as mean and standard deviation. The prevalence of patients' diagnoses was calculated. In the comparison of categorical data, the Pearson Chi-square test was used, and in cases where the variables did not show normal distribution, the Mann-Whitney U test was used for comparisons between variables. Statistical significance was considered at p<0.05 [6,7].
Results
Of our patients, 110 were male, 90 were female (1.22/1). The patients' ages ranged from 6 months to 60 months, with a mean age of 21.82 ± 12.69 months. Most commonly, patients were under 2 years old; 138 patients (69%) were observed in this age group. The average age for each gender was around 18 months.
At birth, 156 patients (78%) were full-term, 120 patients (60%) were born with normal delivery (NSVD), and 38 (19%) had a history of difficult delivery. Family history of FC was present in 50 patients (25%), and a history of epilepsy in 20 patients (10%). Table 1 shows the distribution of the patients' demographic characteristics [8,9].
| n (number of people) | % (percentage ) | ||
| Gender | Male | 110 | 55,0 |
| Female | 90 | 45,0 | |
| Birth week | Borderline preterm (37-38 week) | 24 | 12,0 |
| Term (38-42 week) | 156 | 78,0 | |
| Postterm (>42 week) | 20 | 10,0 | |
| Type of birth | Cesarean section (C/S) | 80 | 39,9 |
| Spontaneous vaginal delivery (NSVD) | 120 | 60,1 | |
| Difficult birth history | No | 162 | 81,0 |
| Yes | 38 | 19,0 | |
| Parental consanguinity | No | 196 | 98,00 |
| Yes | 4 | 2,00 | |
| Family history of epilepsy | No | 180 | 90,00 |
| Yes | 20 | 10,00 | |
| Family history of FC | No | 150 | 75,00 |
| Male | 50 | 25,00 | |
| Note: n: number of people, (%): percentage | |||
Table 1: Distribution of patients according to demographic characteristics.
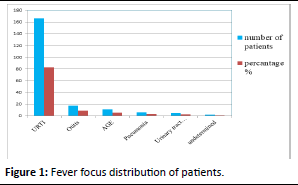
When the foci were exzamined, the most frequently observed focus was URTI in 166 (83.0%) patients. No focus was detected in 2 (1.0%) patients. Lumber Puncture (LP) was performed on these two patients, but no evidence of a Central Nervous System (CNS) infection was found. The distribution of the patients’ fever foci is shown in Figure 1.
Figure 1: Fever focus distribution of patients.
When the follow-up process of patients was examined, it was found that 45 (22.5%) patients experienced recurring seizures, and 26 (13.0%) patients received a diagnosis of epilepsy. Patients who were on continuous antiepileptic treatment had a higher rate of seizure recurrence, while those with tonic-clonic and focal seizure clinics had lower rates compared to other clinics. It was observed that patients with abnormal EEG results had a higher rate of seizure recurrence compared to other clinics (Table 2).
|
|
|
Seizure recurrence |
p* |
|
|
No n (%) |
Yes n (%) |
|||
|
Gender |
Male |
84 (76,4) |
26 (23,6) |
0,670 |
|
Female |
71 (78,9) |
19 (21,1) |
||
|
Age |
Below 1 year old |
39 (70,9) |
16 (29,1) |
0,136 |
|
1-2 years old |
70 (84,3) |
13 (15,7) |
||
|
Above 2 years old |
46 (74,2) |
16 (25,8) |
||
|
Type of birth |
Cesarean section (C/S) |
62 (77,5) |
18 (22,5) |
0,105 |
|
Spontaneous vaginal delivery (NSVD) |
107 (89,2) |
13 (10,8) |
||
|
 Birth week |
Borderline preterm (37-38 week) |
14 (58,4) |
10 (41,6) |
0,134 |
|
Term (38-42 week) |
144 (92,3) |
12 (7,7) |
||
|
Post-term (>42 week) |
18 (90,0) |
2 (10,0) |
||
|
 Difficult birth history |
No |
143 (89,4) |
19 (10,6) |
0,574 |
|
Yes |
35 (92,2) |
3 (7,8) |
||
|
Family history of epilepsy |
No |
138 (76,7) |
42 (23,3) |
0,572 |
|
Yes |
17 (85) |
3 (15) |
||
|
Parental consanguinity |
No |
152 (77,6) |
44 (22,4) |
0,904 |
|
Yes |
3 (75) |
1 (25) |
||
|
Family history of FC |
No |
114 (76) |
36 (24) |
0,379 |
|
Yes |
41 (82) |
9 (18) |
||
|
Body temperature at which the seizure occurred |
Below 38,3 degrees |
90 (75,0) |
30 (25,0) |
0,300 |
|
Above 38,3 degrees |
65 (81,3) |
15 (18,8) |
||
|
 Number of seizures |
1 |
57 (65,0) |
3 (5,0) |
<0,001 |
|
>1 |
98 (70,0) |
42 (60,0) |
||
|
 EEG |
Normal |
97 (75,2) |
5 (9,1) |
0,033 |
|
Abnormal |
8 (50,0) |
32 (24,8) |
||
|
Radiological imaging |
Normal |
50 (80,3) |
18 (26,5) |
0,513 |
|
Abnormal |
3 (60,0) |
2 (40,0) |
||
|
Treatment |
No, antipyretic if necessary |
65 (86,7) |
10 (13,3) |
0,035 |
|
Intermittent rectal diazepam |
12 (80,0) |
3 (20,0) |
||
|
Continuous antiepileptic |
84 (71,2) |
34 (28,8) |
||
|
Febril seizure type |
Simple |
67 (81,7) |
15 (18,3) |
0,689 |
|
Complex |
88 (74,6) |
30 (25,4) |
||
|
Seizure clinic |
Tonic |
7 (100) |
0 (0) |
0,010 |
|
Klonic |
3 (100) |
0 (0) |
||
|
Atonic |
7 (46,7) |
8 (53,3) |
||
|
Tonic klonic |
128 (78) |
36 (22) |
||
|
Focal |
84 (76,4) |
26 (23,6) |
||
|
Note: n: number of patients, (%): percentage, *Ki Square Test. |
||||
Table 2: Comparison of patients' seizure recurrence with other variables.
In patients receiving continuous antiepileptic therapy, a higher rate of epilepsy development was observed. Patients with abnormal EEG results were found to have a higher rate of receiving an epilepsy diagnosis. When comparing the body temperature during seizures, it was found that patients who experienced seizures below 38.3 degrees Celsius had a higher rate of receiving an epilepsy diagnosis. Patients who had multiple seizures also had a higher rate of receiving an epilepsy diagnosis (Table 3).
|
|
|
Development of epilepsy |
p* |
|
|
No n (%) |
Yes n (%) |
|||
|
Gender |
Erkek |
98 (89,1) |
12 (10,9) |
0,331 |
|
Kiz |
76 (84,4) |
14 (15,6) |
||
|
Age |
Below 1 year old |
39 (70,9) |
16 (29,1) |
0,678 |
|
1-2 years old |
70 (84,3) |
13 (15,7) |
||
|
Above 2 years old |
46 (74,2) |
16 (25,8) |
||
|
Type of birth |
Cesarean section (C/S) |
64 (80,0) |
16 (20,0) |
0,072 |
|
Spontaneous vaginal delivery (NSVD) |
108 (90,0) |
12 (10,0) |
||
|
Birth week |
Borderline preterm (37-38 week) |
16 (66,7) |
8 (33,3) |
0,184 |
|
Term (38-42 week) |
145 (92,9) |
11 (7,1) |
||
|
Post-term (>42 week) |
19 (95,0) |
1 (5,0) |
||
|
Difficult birth history |
No |
143 (89,4) |
19 (11,7) |
0,524 |
|
Yes |
35 (87,5) |
3 (7,8) |
||
|
Family history of epilepsy |
No |
156 (86,7) |
24 (13,3) |
0,674 |
|
Yes |
18 (90) |
2 (10) |
||
|
Parental consanguinity |
No |
170 (86,7) |
26 (13,3) |
0,435 |
|
Yes |
4 (100) |
0 (0) |
||
|
Family history of FC |
No |
127 (84,7) |
23 (15,3) |
0,089 |
|
Yes |
47 (94) |
3 (6) |
||
|
Body temperature at which the seizure occurred |
Below 38,3 degrees |
98 (81,7) |
22 (18,3) |
0,004 |
|
above 38,3 degrees |
76 (95,0) |
4 (5,0) |
||
|
Number of seizures |
1 |
57 (95,0) |
3 (5,0) |
0,028 |
|
>1 |
117 (83,6) |
23 (16,4) |
||
|
EEG |
Normal |
117 (90,7) |
12 (9,3) |
<0,001 |
|
Abnormal |
3 (18,8) |
13 (81,3) |
||
|
Radiological imaging |
Normal |
55 (80,9) |
13 (19,1) |
0,265 |
|
Abnormal |
3 (60,0) |
2 (40,0) |
||
|
Treatment |
No, antipyretic if necessary |
73 (97,3) |
2 (2,7) |
0,001 |
|
Intermittent rectal diazepam |
14 (93,3) |
1 (6,7) |
||
|
Continuous antiepileptic |
94 (79,7) |
24 (20,3) |
||
|
Febril seizure type |
Simple |
71 (86,6) |
11 (13,4) |
0,786 |
|
Complex |
103 (87,3) |
15 (12,7) |
||
|
Seizure clinic |
Tonic |
6 (85,7) |
1 (14,3) |
0,689 |
|
Klonic |
3 (100) |
0 (0) |
||
|
Atonic |
13 (86,7) |
2 (13,3) |
||
|
Tonic klonic |
141 (86) |
23 (14) |
||
|
Focal |
11 (100) |
0 (0) |
||
|
Note: n: number of patients, (%): percentage, *Ki Square Test. |
||||
Table 3: Comparison of patients' epilepsy development with other variables.
It was observed that EEGs were conducted for 145 out of 200 patients (72.5%). Among them, 129 (64.5%) showed normal EEG results, while 16 (8%) showed abnormal EEG results. Among the 49 patients (24.5%) with simple febrile convulsions (SFC), abnormal EEG results were found in 5 (2.5%), and among the 96 patients (48%) with complex febrile convulsions (CFC), abnormal EEG results were found in 11 (5.5%). There was no significant relationship found between the type of febrile convulsion and EEG findings (p=0.605) (Table 4).
|
|
Normal EEG n (%) |
Anormal EEG n (%) |
Total n (%) |
P* |
|
Simple FC |
44 (22) |
5 (2,5) |
49 (24,5) |
0,605 |
|
Complex FC |
85 (42,5) |
11 (5,5) |
96 (48) |
|
|
Total |
129 (64,5) |
16 (8) |
145 (72,5) |
|
|
Note: n: number of patients, (%): percentage, *Ki Square Test. |
||||
Table 4: Evaluation of EEG findings according to the type of febrile convulsion.
Patients with recurrent seizures were found to have higher CRP (C-Reactive Protein) and platelet levels compared to patients with epilepsy. No relationship was found between other laboratory values and the development of epilepsy (Tables 5 and 6).
|
|
|
Seizure recurrence |
||
|
Yok n (%) |
Var n (%) |
p* |
||
|
C-reaktif protein |
Normal |
98 (77,2) |
29 (22,8) |
0,881 |
|
High |
57 (78,1) |
16 (21,9) |
||
|
White blood cells |
Low |
16 (72,7) |
6 (27,3) |
0,772 |
|
Normal |
125 (77,6) |
36 (22,4) |
||
|
High |
14 (82,4) |
3 (17,6) |
||
|
Neutrophil count |
Low |
7 (77,8) |
2 (22,2) |
0,286 |
|
Normal |
118 (76,1) |
37 (23,9) |
||
|
High |
30 (83,3) |
6 (16,7) |
||
|
Hemoglobin |
Low |
57 (76) |
18 (24) |
0,694 |
|
Normal |
98 (78,4) |
27 (21,6) |
||
|
MCV |
Normal |
63 (77,8) |
18 (22,2) |
0,177 |
|
High |
92 (78) |
26 (22) |
||
|
Platelet count |
High |
2 (28,5) |
5 (71,5) |
0,009 |
|
|
low/normal |
122 (78,2) |
34 (21,8) |
|
|
Note: n: number of patients, (%): percentage, *Ki Square Test |
||||
Table 5: Comparison of laboratory variables with patients' seizure recurrence.
|
|
|
Development of epilepsy |
||
|
No n (%) |
Yes n (%) |
p* |
||
|
C-reaktif protein |
Normal |
106 (83,5) |
21 (16,5) |
0,049 |
|
High |
68 (93,2) |
5 (6,8) |
||
|
White blood cells |
Low |
18 (81,8) |
4 (18,2) |
0,526 |
|
Normal |
140 (87) |
21 (13) |
||
|
High |
16 (94,1) |
1 (5,9) |
||
|
Neutrophil count |
Low |
9 (100) |
0 (0) |
0,881 |
|
Normal |
132 (85,2) |
23 (14,8) |
||
|
High |
33 (91,7) |
3 (8,3) |
||
|
Hemoglobin |
Low |
65 (86,7) |
10 (13,3) |
0,914 |
|
Normal |
109 (87,2) |
16 (12,8) |
||
|
MCV |
Normal |
75 (92,6) |
6 (7,4) |
0,647 |
|
High |
98 (83,1) |
20 (16,9) |
||
|
Platelet count |
High |
7 (100) |
0 (0) |
0,355 |
|
low/normal |
134 (85,9) |
22 (14,1) |
||
|
Note: n: number of patients, (%): percentage, *Ki Square Test. |
||||
Table 6: Comparison of laboratory variables with patients' development of epilepsy.
A statistically significant relationship was found between the development of epilepsy during follow-up and the body temperature at which seizures occurred and the number of seizures (p=0,048, p<0,001). It has been determined that in patients who develop epilepsy, the body temperature value at which seizures occur is lower and also the number of seizures is 3 or more. No statistically significant relationship was found between the development of epilepsy during follow-up and the duration of seizures, the age of the patient, and the age at which the irst seizure occurred (Table 7).
|
|
Development of epilepsy (no) |
Development of epilepsy (yes) |
p* |
||
|
Mean ± standard deviation |
Median |
Mean ± standard deviation |
Median |
||
|
Body temperature |
38,4 ± 0,6 |
38 |
38,2 ± 0,5 |
38 |
0,048 |
|
Number of seizures |
2,1 ± 1,2 |
2 |
3,3 ± 1,9 |
3 |
<0,001 |
|
Duration of seizure |
8 ± 8,5 |
5 |
4,9 ± 6,9 |
3 |
0,091 |
|
Age (months) |
45 ± 25,6 |
44 |
54 ± 27,1 |
57 |
0,081 |
|
Seizure age (months) |
22,1 ± 13 |
18 |
20,2 ± 10,8 |
18 |
0,575 |
|
Note: *Mann Whitney U test. |
|||||
Table 7: Comparison of patients' development of epilepsy with other factors.
Discussion
Febrile Convulsions (FC) are the most common neurological problem in childhood and the most frequently encountered type of convulsion. Although they generally have a favorable prognosis, they can recur and evolve into afebrile seizures. Therefore, understanding predisposing factors is of great importance.
FC is more commonly observed in boys compared to girls. In studies conducted abroad and in our country, the male-tofemale ratio has been reported as 1.3/1 and 1.36/1 respectively [8, 9]. In our study with 200 patients, a similar male-to-female ratio of 1.22/1 was found.
Genetic factors are known to play a significant role in FC. However, the complete genetic transmission remains unclear. In studies conducted abroad and in our country, a history of FC among first-degree relatives has been found to be 26.6% and 20.8% respectively [10,11]. In our study, the frequency of FC among first-degree relatives was found to be 25%, similar to the literature.
The accepted fever threshold in FC has been reported as axillary 38°C in one group of studies, and 38.5°C and above in another group. In our study, the body temperature ranged from 37.5°C to 40°C, with an average of 38.3°C. It was found that 120 patients (60%) had seizures at temperatures below 38.3°C, and in this group, the risk of developing epilepsy was significantly higher [12,13].
The source of fever in febrile convulsions is often viral infections such as Upper Respiratory Tract Infections (URTI), pharyngitis, Urinary Tract Infections (UTI), Acute Otitis Media (AOM), pneumonia, roseola infantum, and non-infectious diseases. In the study by Abuekteish et al. involving 203 patients, URTI was reported as the fever focus in 53% of cases, while in the study by Öztürk et al., this rate was 75.8%. Similarly, in our study, URTI was most frequently detected at a rate of 83%, consistent with the literature.
In the study by Verrotti et al.s, Complex Febrile Convulsions (CFC) were found in 27.2% of cases, and in the study by Kolfen, they were found in 22.5% of cases. Ling reported that 90% of seizures in his study and Knugsen reported 96% of seizures lasted less than 15 minutes. In our study, the number of cases with CFC was found to be 105 (52.5%). This result may be due to our institution being a tertiary care center, where complicated and recurring cases are referred or transferred from lower-level healthcare facilities. Among the CFC cases in our study, 85 (80.9%) had recurrence within 24 hours, 22 (20.9%) lasted longer than 15 minutes, 9 (8.6%) had focal seizures, and 2 (1.9%) were diagnosed as complex due to both focal seizures and lasting longer than 15 minutes [14-16].
In previous studies, imaging tools such as EEG, MRI, and BBT have been found to be largely normal in children with Febrile Convulsions (FC), and they were concluded to not be associated with recurrence or development of epilepsy. In our study, imaging was performed on 73 patients, of whom 15 patients received a diagnosis of epilepsy. Pathology was detected in the imaging of 2 patients who also developed epilepsy during follow-up. Patients with abnormal EEG results were found to have a higher rate of receiving an epilepsy diagnosis [17,18].
Previous studies have suggested a relationship between convulsions triggered by different mechanisms of the immune system and elevated acute-phase reactants such as CRP, which are indicators of inflammation, with epilepsy. Another study found that thrombocytosis, seen as an acute-phase reactant, was also associated with febrile seizures, and IL-6 levels and platelet levels were found to be higher in febrile seizure patients compared to the control group [19]. In our study, patients with recurrent seizures were found to have higher levels of CRP and platelets compared to patients with epilepsy.
Both simple and complex febrile convulsions have shown a higher recurrence rate in patients receiving treatment compared to those who did not receive treatment. One treatment option is continuous use of antiepileptic drugs [20]. reported in their study that phenobarbital, diazepam, phenytoin, and antipyretics did not show significant superiority in preventing FC recurrence attacks over each other. In our study, a recurrence rate of 28.8% was observed in patients using long-term antiepileptic drugs. There was no statistically significant relationship found between seizure recurrence and development of epilepsy based on the type of treatment received.
Our study had some limitations. A majority of our patients had complex febrile convulsions, which differs from the data in the literature. Based on the data we analyzed, we believe that some patients' seizures were terminated in the emergency department after admission, hence their duration was recorded as <5 minutes. However, according to the literature, seizure recurrence and epilepsy are directly proportional to seizure duration. We attribute this to providing information to families for seizure management and termination of seizures in the emergency department for some cases, resulting in shorter durations. Additionally, no relationship was found between family history of FC recurrence and epilepsy in our region. We believe this may be due to healthcare providers and families in our region providing more appropriate follow-up and treatment during febrile illness periods, potentially raising the threshold for experiencing FC.
In the literature, the role of sodium channels in the pathogenesis of epilepsy and FC is mostly mentioned, and in addition, some studies have pointed out the relationship between FEB gene loci and related syndromes. On the other hand, the condition known as Dravet Syndrome may be mistakenly perceived as FC. Dravet Syndrome should be considered if afebrile focal seizures and myoclonies are added to febrile seizures and negatively affect the child's mental functions over time.
SCN1A gene analysis should be used, especially in the presence of prolonged and lateralized febrile seizures. If a mutation is detected, the diagnoses of GEFS+, typical or borderline Dravet Syndrome should be reviewed, taking into account the patient's clinic.We believe that with the data obtained as a result of comprehensive epidemiological and genetic studies, the data currently available in the literature will solidify and illuminate the role of genetic predisposition in the etiopathogenesis of FC in the future.
Conclusion
Febrile convulsions are the most common type of convulsion in childhood. Although they generally have a benign course, they can recur and transform into afebrile seizures. Therefore, understanding predisposing factors is crucial. Despite being considered a benign condition, the high frequency of recurrence and increased risk of epilepsy compared to the general population necessitates careful monitoring. Since follow-up is mostly conducted in primary and secondary healthcare settings, careful examination for epilepsy risk factors is essential.
References
- Hirtz D (1997) Febrile seizures. Pediatr Rev 18:5-9
- Subcommittee on Febrile Seizures (2011) Febrile seizures: guideline for the neurodiagnostic evaluation of the child with a simple febrile seizure. Pediatrics 127:389-394
- Yayla V, Çakmak G, Apak Ä°, AteÅ? U, ErdoÄ?an F (1997) Ä°lkokul çocuklarında geçirilmiÅ? febril konvülsiyon prevelansı. Yeni Sempozyum 35:11-13
- Stanhope JM, Brody JA, Brink E, Morris CE (1972) Convulsions among the Chamorro people of Guam, Mariana Island. Febrile convulsions. Am J Epidemiol 95:299-304
- Canpolat M, Per H, GümüÅ? H, ve arkadaÅ?ları (2013) Kayseri ili febril konvülsiyon prevalansının araÅ?tırılması; Febril konvülsiyon rekürrensi ve epilepsi geliÅ?imi için risk faktörlerinin belirlenmesi. XV 93-94
- Erdil A, Tan H, Turan M, Küçükaslan Ä° (2016) Erzurum il merkezinde çocuklarda febril konvülziyon prevalansı. Türkiye Klinikleri J Pediatr 25:67-73
- Vetterlein MW, Meyer CP, Leyh-Bannurah SR, Mayr R, Gierth M, et al. (2017) Effect of hospital and surgeon case volume on perioperative quality of care and short-term outcomes after radical cystectomy for muscle-invasive bladder cancer: Results from a European tertiary care center cohort. Clin Genitourin Cancer 15:e809-e817
[Crossref] [Google Scholar] [PubMed]
- Okumura A, Uemura N, Suzuki M, Itomi K, Watanabe K (2004) Unconsciousness and delirious behavior in children with febrile seizures. Pediatr Neurol 30:316-319
- Ozmen M, Caliskan M (1995) Febrile convulsions. Turk Pediatr Arch 30
- Ling SG (2000) Febrile convulsions: Acute seizures characteristics and anti-convulsant therapy. Ann Trop Pediatr 20:227-230
- Yılmaz Ü, Özdemir R, Çelik T, Berksoy EA (2014) Clinical and paraclinical features in children with febrile seizures. Dicle Medical Journal/Dicle Medical Journal 41:156-162
- Abuekteish F, Daoud AS, al-Sheyyab M, Nou’man M (2000) Demographic characteristics and risk factors of first febrile seizures: a Jordanian experience. Trop Doct 30:25-27
- Öztürk MK, Önal AE, Tümerdem Y (2002) Prevelance of febrile convulsions in a group of children aged 0 to 9 years in a slum in Ä°stanbul. Med Bull Ä°stanbul 35:79-84
- Verrotti A, Latini G, di Corcia G, Giannuzzi R, Salladini C, et al. (2004) Intermittent oral diazepam prophylaxis in febrile convulsions: its effectiveness for febrile seizure recurrence. Eur J Ped Neurol 8:131-134
- Kölfen W, Pehle K, König S (1998) Is the long-term outcome of following febrile convulsions favorable? Dev Med Child Neurol 40:667-671
- Knudsen FU (2000) Febrile seizures: treatment and prognosis. Epilepsia 41:2-9
- Sofijanov N, Emoto S, Kuturec M, Dukovski M, Duma F, et al. (1992) Febrile seizures: clinical characteristics and initial EEG. Epilepsia 33:52-57
- Biçer S, Arslan G, Yılmaz Ç, Öztürk S, Aktay N, et al. (2003) Febril konvülziyonlar: Klinik ve risk faktörleri. Göztepe Tıp Derg 18:88-91
- Li G, Bauer S, Nowak M, Norwood B, Tackenberg B, et al. (2011) Cytokines and epilepsy. Seizure 20:249–256
- Offringa M, Hazebroek-Kampschreur AAJM, Derksen-Lubsen G (1991) Prevalence of febrile seizures in Dutch school children. Paediatr Perinat Epidemiol 5:181–188
Open Access Journals
- Aquaculture & Veterinary Science
- Chemistry & Chemical Sciences
- Clinical Sciences
- Engineering
- General Science
- Genetics & Molecular Biology
- Health Care & Nursing
- Immunology & Microbiology
- Materials Science
- Mathematics & Physics
- Medical Sciences
- Neurology & Psychiatry
- Oncology & Cancer Science
- Pharmaceutical Sciences