ISSN : 2576-3911
Integrative Journal of Global Health
Association of Vitamin D Deficiency and Acute Coronary Syndrome Our Experience
Mohanty Bijaya*, K Shiva Kumar and Prasad Satish
Department of Medicine, Tata Main Hospital, Jamshedpur, India
- *Corresponding Author:
- Bijaya M
Consultant, Department of Medicine
Tata Main Hospital, Jamshedpur, India
Tel: 7763807140
E-mail: bijayamohantytmh@gmail.com
Received date: February 28, 2018; Accepted date: March 26, 2018; Published date: March 28, 2018
Copyright: © 2018 Bijaya M. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Introduction
Despite progress in the prevention of cardiovascular diseases, a significant proportion of first cardiovascular events occur among individuals without traditional risk factors. The advancement of pathophysiology of atherosclerotic vascular diseases has brought new insight regarding potential indicators of underlying hidden atherosclerosis and cardiovascular risk. Recently attention has been focused on various novel inflammatory markers, especially vitamin D. Particularly a growing body of evidence has identified vitamin D deficiency as a potential risk factor for acute coronary syndrome. The research revealed that vitamin D receptor (VDR) was identified in almost all human cells. Relationship between the cardiovascular system system and vitamin D status was first demonstrated in a study on a rat model deficient in vitamin D more than 20 years ago. Vitamin D has antiatherosclerotic, anti-inflammatory and direct cardio-protective actions. Studies report an inverse relationship between levels of vitamin D and atherosclerotic calcification. Also. vitamin D levels are correlated with other coronary heart disease risk factors, such as hypertension, hyperlipidemia and diabetes. So, the association between vitamin D deficiency and ischaemic heart disease may occur directly or indirectly by influencing the risk factors for ACS. Vitamin D supplementation has been shown to have a protective effect in limited studies of, but further research is needed. We have undertaken this study in our hospital with the aim to identify the relation between vitamin D levels with acute coronary syndrome.
Materials and Methods
This is a hospital based prospective study. Patients coming to emergency with chest pain, diagnosed as acute coronary syndrome and admitted in medical wards and ICU were included in this study with their informed consent. This study was conducted in Tata Main Hospital, Jamshedpur, Jharkhand which is 940 bedded multidisciplinary hospital. The study was conducted over a period of one and half years from January 2013 to June 2014 (18 months). Sample consists of 100 cases of acute coronary syndromes and randomly selected 100 age and sex matched controls written consent was taken from each patient/relative and studied according to predesigned proforma after approval of Ethics committee.
Patients with ST elevation acute myocardial Infarction (STEMI), unstable angina and non-ST elevation myocardial infarction (NSTEMI) were included in the study. Diagnosis of acute coronary syndromes was made by history, physical examination, electrocardiogram and CK-MB levels (more than three times the normal limits). Patients with malabsorption syndromes, chronic liver disorder, chronic renal disease, type 2 diabetes mellitus, rickets, osteomalacia, on vitamin D therapy, severe protein energy malnutrition and intake of drugs like PTH analogues were excluded from the study. Data collection was done by direct anthropometric measurements (weight, height, waist circumference, and BMI) and biochemical tests (serum Vitamin D level, serum creatinine, liver function tests, cardiac enzymes and lipid profile). The indirect method used a structured face to face questionnaire. The questionnaire was prepared to include more variables in relation to the objectives of the study. The main components of the questionnaire were personal demographic and socioeconomic data including gender, age, marital status, occupation. Clinical assessment consisting of participants’ family history of ischaemic heart disease and/or hyperlipidemia, medical history of conditions predisposing to coronary artery disease and lifestyle factors like smoking and physical activity level was done. Clinical examination was conducted for both, patients and controls to prove or rule out ACS and included: participants’ family history, medical history of conditions predisposing to ACS, drug history, and detail physical examination., a 12 lead ECG, 2D echocardiography done in all cases to prove ACS.
Observation and results
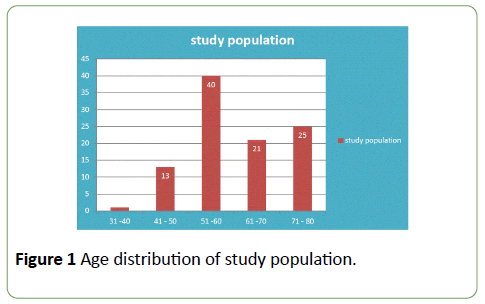
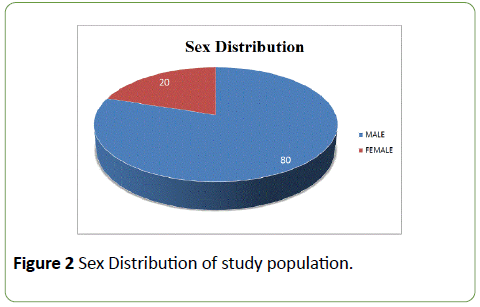
Maximum incidence of acute coronary syndrome was observed in age group between 51 to 60 years, accounting for 40% patients (Figure 1). 80% patients were male and 20% were female (Figure 2). Mean age of incidence in male was 59.9 years and that for female 64.2 years.
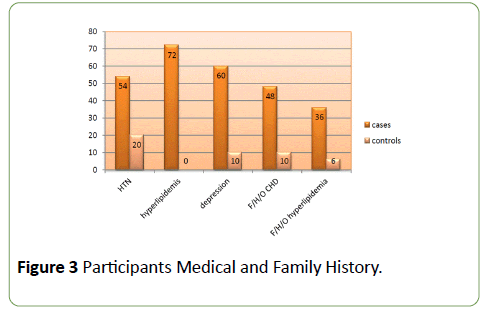
Analysis of participant’s medical and family history revealed that 54% of ACS patients were hypertensive while 20% of the control were hypertensive. 72% of ACS cases had associated hyperlipidemia, while none of the controls had hyperlipidemia and 60% of ACS cases suffered from depression compared to 10% of controls which are statistically significant (P value=0.00001) (Figure 3). The study shows that 48% of ACS patients had a positive family history of ACS while 10% of healthy participants had this feature the difference was statistically significant. Family history of hyperlipidemia was present among 36% of ACS patients compared to 6% of controls, a result that was statistically significant (P value=0.00001).
Figure 3: Participants Medical and Family History.
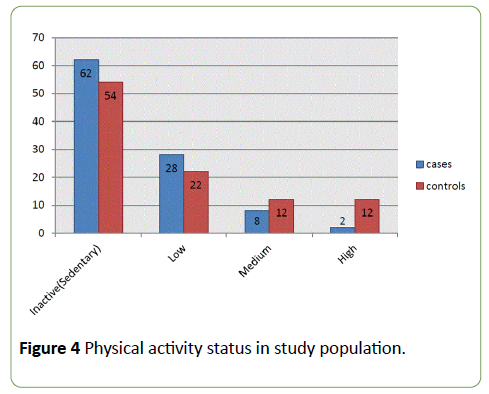
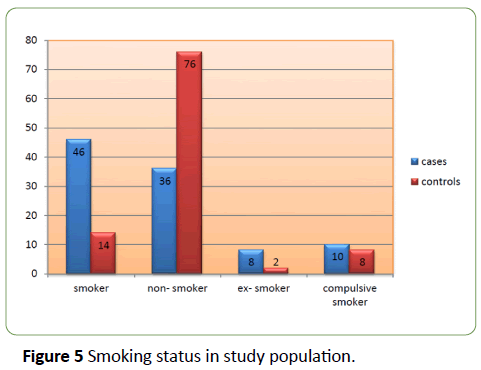
Comparison of lifestyle factors revealed that (Figure 4 and 5) 46% of cases were active smokers compared to 14% of controls out of which 10% of ACS cases were compulsive smokers in comparison with 8% of controls. Differences reached statistical significance (P-value<0.001). Regarding physical activity level, 62% and 28% of ACS cases were sedentary and low level active respectively, compared to 54% and 22% of controls. Activity levels were measured according to U.S. Department of Health and Human Services (U.S. HHS 2008), Physical Activity Guidelines for Americans.
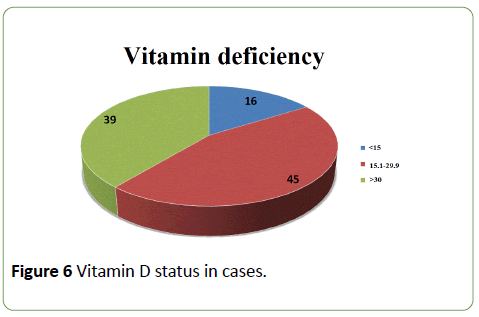
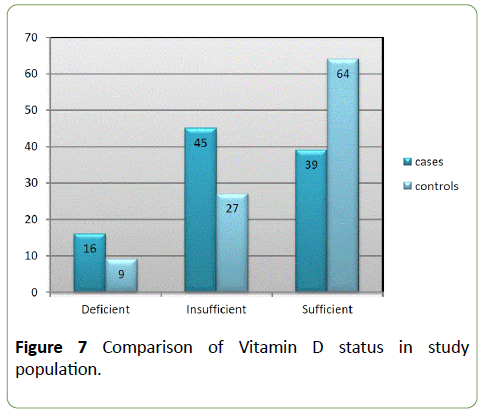
Using BMI as indicator, obesity was present in 56% of ACS cases compared to 44% in controls. Abdominal obesity (using waist circumference) among men was present in 75% of cases and 31.2% of controls. The differences reached statistical significance (P-value=0.00001). Abdominal obesity in women was present in the same proportion (80%) among the cases and controls Comparison of Serum Vitamin D levels in study participants was done. (Table 1, Figures 6 and 7).
| Vitamin D3 levels | Cases | Controls | Total | P value |
|---|---|---|---|---|
| Deficient (<15) | 16 | 9 | 25 | 0.001 |
| Insufficient (16-30) | 45 | 27 | 72 | 0.001 |
| Sufficient (>30) | 39 | 64 | 103 | 0.001 |
| Total | 100 | 100 | 200 | - |
Table 1: Comparison of serum level of Vitamin D in nanogram/dl.
Average serum vitamin D level in ACS patients was 28.30 ng/ml and 32.97 ng/ml in controls, which represented a statistically significant difference (P=0.004). In study population, 16% of ACS patients were vitamin D3 deficient, 45% of ACS patients were vitamin D insufficient while only 9% of healthy participants were vitamin D3 deficient, 27% of controls vitamin D3 insufficient. The chi-square statistic is 12.528. The P-Value is 0.001. The result is significant at p<0.05.
Comparison of the exposure to sun between the two study groups shows that 80% of ACS patients and 84% of controls had sufficient sun exposure which is defined as approximately 5-30 minutes of sun exposure between 10 AM and 3 PM at least twice a week to the face, arms, legs, or back without sunscreen that usually lead to sufficient vitamin D synthesis in human skin.
Discussion
In our series 80% were male and 20% were female which is similar to study by Foussas et al with 79% male [1] and Mohmoud Suleiman et al. study with male predominance too [2]. Of all participants in this study, most were in 50-60-year age group which is consistent with the report of NHLBI (National Heart, Lungs and Blood Institute) in 2011. In Foussas et al. study and Mohmoud Suleiman et al. [1,2] study patients were in seventh decade. In Indian subcontinent coronary artery diseases occur a decade earlier than the western population. So, mean age of our patients is comparable to above mentioned studies. This study found a statistically significant positive association between active smoking and acute coronary syndrome. This result is supported by AHA (American Heart Association) 2013) which stated that smokers' risk of developing coronary artery disease is 2-4 times that of nonsmokers. WHF (Women heart foundation) in 2013 also specified that smoking is estimated to cause nearly 10% of all acute coronary syndromes. In Foussas et al. study, smoking was observed in 57% of patients. In Mohmoud Suleiman et al. study, smoking was observed in 40% of patients which is quite similar to ours which observed 46% of smokers having features of coronary artery disease, where as in Prof. Salim Yusuf et al study (65.19% of patients were smokers. Our study showed that people who are physically active are at lower risk of ACS. This study revealed that more cases than controls had a positive family history of coronary artery disease which is in accord with many other studies. Roeters van Lennep et al. [3] found that individuals with a positive family history have an increased risk of premature coronary events. The study also showed a statistically significant positive association between hypertension and ACS. In Foussas et al study hypertension was seen in 51% of patients and in Mohmoud Suleiman et al study in 53% of patients. In “INTER HEART” study by Prof. Salim Yusuf et al. [4] hypertension was seen in only 19.3% of patients.
Average level of 25(OH) Vitamin D in our study participants was 30.67 ng/ml. Average serum vitamin D level in ACS patients was lower (28.30 ng /ml) than the healthy participants (32.97 ng/ml) which is statistically significant. Pilz et al [5] showed that risk of cardiovascular mortality was significantly increased in individuals with low 25(OH) D levels. A community-based case-control study in New Zealand found that men with myocardial infarction had lower levels of 25(OH)D compared to controls. Among the Framingham Offspring Study in individuals free of cardiovascular disease, those with 25(OH)D levels less than 15 ng/ml had an increased risk of increased coronary events. Lavie et al. [6] while evaluating patients admitted with acute coronary syndrome also found that most patients had low vitamin D levels.
In a study by Lund et al. [7], vitamin D levels were measured in 128 patients with ischemic heart disease admitted to the Frederiksberg Hospital in Denmark. 53 of these patients had a diagnosis of acute myocardial infarction and 75 had angina pectoris. The mean vitamin D levels in the AMI and angina patients were 24 ± 10 ng/ml and 23.5 ± 9.6 ng/ml respectively. The mean vitamin D levels in the cases were lower compared to the controls in the months of May-June (P<0.01) and July- August (P<0.05), indicating that serum vitamin D levels change with sun exposure. In a prospective study conducted by Edward Giovannucci et al. [8] which was a nested case control study included 18, 225 health professionals. Follow up study concluded that low levels of vitamin D are associated with higher risk of myocardial infarction. In a cross-sectional study conducted by Zahra Dana Siadat et al. [9] also observed low levels of Vitamin D in coronary artery disease. Wang et al. also observed the same [10-16]. However, in their study levels lower than 15 ng/ml were considered as vitamin D deficiency while we considered levels lower than 30 ng/ml as vitamin D deficiency. Similar results were found by Scragg et al. [10] in Central Auckland area of New Zealand [17-24].
Limitations of the study
• This is a hospital based small study of a short duration [25-29].
• This study limits the conclusion about the mechanism and temporal association [30-33]. A prospective study with follow up evaluation of mortality would have helped to evaluate the role of vitamin D deficiency as cardiovascular risk factor [34,35].
Conclusions
In the current study we observed an inverse association between acute coronary syndrome and vitamin D deficiency. Since Vitamin D deficiency is a potentially modifiable risk factor people with cardiovascular risk factors should be screened and treated accordingly. Patients getting admitted with acute coronary syndrome should be evaluated for vitamin D deficiency and accordingly supplementation should be recommended. Even the family members of patients should be explained regarding vitamin D in today’s perspective.
References
- Foussas SG, Zairis MN, Lyras AG, Patsourakos NG, Tsirimpis VG, Katsaros K et al. Early prognostic usefulness of C reactive protein added to thrombolysis in myocardial infarction risk score in acute coronary syndromes. Am J Car 2005; 96: p 533-7.
- Suleiman M, Aronson D, Reisner SA, Kapeliovich MR, Markiewicz W, Levy Y et al. Admission C reactive protein levels and 30-day mortality in patients with acute myocardial infarction. Am J of Med. 2003 Dec 15; 115 (9): p 735-7.
- Roeters van Lennep J.E., Westerveld H. T., Erkelens D.W., van der Wall E.E. Risk factor for coronary heart disease: implications of gender.Cardiovascular Research 2002; 53: 538–549.
- Yusuf S, Hawken S, Ounpuu S, Dans T, Avezum A, Lanas F et al. Effect of potentially modifiable risk factors associated with myocardial infarction in 52 countries (the INTERHEART study): a case control study. Lancet. 2004; 364: 937-952.
- Pilz S., Tomaschitz A., Marz W., Drechsler C., Ritz E., Zittermann A.,et al. Vitamin D, cardiovascular disease and mortality. Clin Endocrinol 2011; 75: 575–584.
- Lavie, C.J., Lee, J.H., Milani, R.V. Vitamin D and Cardiovascular Disease. J Am coll cardiol 2011; 58:1547–56.
- Lund B, Badskjaer J, Soerensen OH. Vitamin D and ischaemic heart disease. Horm Metab Res 1978;10:553-6.
- Edward Giovannucci, Yan Liu, Bruce W. Hollis, Eric B. Rimm. 25-Hydroxyvitamin D and Risk of Myocardial Infarction in Men. Arch Intern Med 2008;168(11):1174-80.
- .Zahra Dana Siadat, Keyvan Kiani, Masoumeh Sadeghi, Amir Sina Shariat, Ziba Farajzadegan, Maryam Kheirmand . Association of vitamin D deficiency and coronary artery disease with cardiovascular risk factors. J Res Med Sci 2012; 17(11): 1052–5.
- Scragg R, Jackson R, Holdaway IM, Lim T, Beaglehole R. Myocardial infarction is inversely associated with plasma 25-hydroxyvitamin D3 levels: a community-based.Scragg R, Shaw KT, Murphy S. Effect of winter oral vitamin D3 supplementation on cardiovascular risk factors in elderly adults. Eur J Clin Nutr 1995;49:640-6.
- Klein, S., Allison B.D., Heymsfield B.S., Kelley E.D., Leibel L.R., Nonas, C., et al. 2007. Waist circumference and cardiometabolic risk: a consensus statement from Shaping America’s Health:Association for Weight Management and Obesity Prevention; NAASO, The Obesity Society; the American Society for Nutrition; and the American Diabetes Association. Am j clin nutr 2007;85:1197–202.
- Wang TJ, Pencina MJ, Booth SL, Jacques PF, Ingelsson E, Lanier K et al. Vitamin D deficiency and risk of cardiovascular disease. Circulation. 2008;117:503–11.
- Christakos S, Ajibade WV, Dhawan P, Fechner AJ, Mady LJ. Vitamin D: metabolism. Endocrin Metab Clin. 2010;39:243-53.
- Holick MF. Vitamin D: A millennium perspective. J Cell Biochem 2003;88:296 – 307.
- Brot C, Vestergaard P, Kolthoff N, Gram J, Hermann AP, Sorensen OH. Vitamin D status and its adequacy in healthy Danish perimenopausal women: relationships to dietary intake, sun exposure and serum parathyroid hormone. Br J Nutr 2001;86:S97– 103.
- Lee JH, O’Keefe JH, Bell D, Hensrud DD, Holick MF. Vitamin D deficiency: an important, common, and easily treatable cardiovascular risk factor? J Am Coll Cardiol 2008;52:1949 –56.
- Abuannai M, O’Keefe JH. Vitamin D and cardiovascular health. Primary Care Cardiovasc J 2011;4:59–62.
- Bischoff-Ferrari HA, Giovannucci E, Willett WC, Dietrich T, Dawson-Hughes B. Estimation of optimal serum concentrations of 25-hydroxyvitamin D for multiple health outcomes. Am J Clin Nutr 2006;84:18 –28.
- Cheng S, Massaro JM, Fox CS. Adiposity, cardiometabolic risk, and vitamin D status: the Framingham Heart Study. Diabetes 2010; 59:242– 8.
- 20.Rajakumar K, Fernstrom JD, Holick MF, Janosky JE, Greenspan SL. Vitamin D status and response to vitamin D(3) in obese vs. non-obese African American children. Obesity (Silver Spring) 2008;16:90 –5.
- Binkley N, Novotny R, Krueger D. Low vitamin D status despite abundant sun exposure. J Clin Endocrinol Metab 2007;92:2130 –5.
- Fiscella K, Franks P. Vitamin D, race, and cardiovascular mortality: findings from a national US sample. Ann Fam Med 2010;8:11– 8.
- Wang TJ, Zhang F, Richards JB. Common genetic determinants of vitamin D insufficiency: a genome-wide association study. Lancet 2010;376:180–8.
- Zittermann A, Schleithoff SS, Koerfer R. Putting cardiovascular disease and vitamin D insufficiency into perspective. Brit J Nutr 2005;94:483-92.
- Verhave G, Siegert CEH. Role of vitamin D in cardiovascular disease. Neth J Med 2010;68(3):113-8.
- Parker J, Hashmi O, Dutton D, Mavrodaris A, Stranges S, Kandala NB, et al. Level of vitamin D and cardiometabolic disorders: Systematic review and meta-analysis. Maturitas 2010;65:225-36.
- Lind L, Pollare T, Hvarfner A, Lithell H, Sorensen OH, Ljunghall S. Long-term treatment with active vitamin D (alphacalcidol) in middle-aged men with impaired glucose tolerance. Effects on insulin secretion and sensitivity, glucose tolerance and blood pressure. Diabetes Res 1989;11:141-7.
- Scragg R, Holdaway I, Jackson R, Lim T. Plasma 25-hydroxyvitamin D3 and its relation to physical activity and other heart disease risk factors in the general population. Ann Epidemiol 1992;2(5):697-703.
- Vanga SR, Good M, Howard P, Vacek JL. Review: Vitamin D in cardiovascular health. Am J Cardiol 2010;106(6):798-805.
- Lee JH, O’Keefe JH, Bell D, Hensrud DD, Holick MF. Vitamin D deficiency: an important, common, and easily treatable cardiovascular risk factor? J Am Coll Cardiol 2008;52:1949 –56.
- Zittermann A. Vitamin D and disease prevention with special reference to cardiovascular disease. Prog Biophys Mol Biol 2006;92:39–48.
- Yusuf S, Hawken S, Ounpuu S, Dans T, Avezum A, Lanas F et al. Effect of potentially modifiable risk factors associated with myocardial infarction in 52 countries (the INTERHEART study): a case control study. Lancet. 2004; 364: 937-952.
- Roeters van Lennep J.E., Westerveld H. T., Erkelens D.W., van der Wall E.E. Risk factor for coronary heart disease: implications of gender.Cardiovascular Research 2002; 53: 538–549.
- Lavie, C.J., Lee, J.H., Milani, R.V. Vitamin D and Cardiovascular Disease. J Am coll cardiol 2011; 58:1547–56.
- Wang TJ, Pencina MJ, Booth SL, Jacques PF, Ingelsson E, Lanier K et al. Vitamin D deficiency and risk of cardiovascular disease. Circulation. 2008;117:503– 11.
Open Access Journals
- Aquaculture & Veterinary Science
- Chemistry & Chemical Sciences
- Clinical Sciences
- Engineering
- General Science
- Genetics & Molecular Biology
- Health Care & Nursing
- Immunology & Microbiology
- Materials Science
- Mathematics & Physics
- Medical Sciences
- Neurology & Psychiatry
- Oncology & Cancer Science
- Pharmaceutical Sciences