Keywords
Maldigestion-malabsorption; Defecation; Chronic gastrointestinal disease
Introduction
Dietary therapy is a major component in the management of most gastrointestinal (GI) diseases with compromised digestion and/or absorption. Dietary intervention should be aimed at reducing intestinal inflammation and controlling clinical signs (e.g., vomiting, diarrhea) while providing adequate nutrients to meet requirements, compensate for losses through the GI tract, and promote healing and recovery [1]. Because of the diverse causes resulting in maldigestion-malabsorption, a number of food types may be appropriate [2]. The most commonly used strategy is to feed a highly digestible, low-residue food. Indeed, highly digestible foods favor a more complete nutrient absorption in the proximal gut, thus reducing osmotic diarrhea and uncontrolled fermentation in the distal gut [3,4].
As strict carnivores, cats have naturally limited capacity to digest carbohydrates, and carbohydrate digestion may be more impacted in case of intestinal and/or pancreatic failure. On the contrary, protein and fat digestion is efficient in this species. Studies have demonstrated that high-fat diets are well tolerated in cats with inflammatory bowel disease [5]. Moreover, as fat is high in energy, higher fat foods allow smaller amounts of food intake to maintain energy provision, which minimizes GI work and helps control clinical signs such as restoration of body condition [6].
Fat and protein, especially of animal origin, also improve food palatability which is important in patients with digestive disorders: the unpalatability of low fat – low protein diet could be counterproductive if sick animals refuse to eat it. That is why a highly digestible high protein - low carbohydrate – high fat diet should ideally be proposed to help manage GI diseases in cats. In some cases, increasing dietary fibers may be beneficial for GI tract recovery [5]. Fermentable soluble fibers, including fructooligosaccharides, act as prebiotics and influence positively the composition of the intestinal microbiota. In addition, bacterial fermentation of such fibers increases the concentration of short chain fatty acids (SCFA), mainly butyrate, which have a trophic role and will increase colonocyte growth and proliferation [7,8]. Mucilaginous fibres, with their water-holding capacity, form gels in water and help improve the consistency of the faeces [9-11]. Insoluble fibers can help normalize motility [12].
Supplementation in some specific functional ingredients has also shown various benefits on GI health: exogenous source of free nucleotides, precursor units of DNA and RNA, may optimize the GI function by promoting mucosa renewal and by stimulating local immunity. Clays may also be used: they form a protective film on the digestive mucosa and separate it from the potential irritating or toxic elements in the lumen [13-16].
A new dry diet was developed, combining a specific nutrient profile (high protein – low carbohydrate – high fat) and the supplementation in various functional ingredients with targeted action on the intestinal tract. The objective of this study was to evaluate the clinical efficacy of this diet for the management of chronic maldigestion-malabsorption in cats.
Materials and Methods
Animals
Forty-seven adult client-owned cats were recruited in a database prepared by an independent company specialized in customer surveys. They have experienced chronic continuous or intermittent gastrointestinal disorders of nonspecific causes for minimum 3 months, without deterioration of their general health status. For inclusion, minimum 2 of the 5 following digestive parameters had to be considered as abnormal: frequency of defecation (≥ 3 stools/day), faecal score (≥ 3 using a five-point scoring system where 1=hard dry and crumbly and 5=watery) shown in Figure 1, faeces odour (≥ odorous=slightly bearable) (Table 1), faeces quantity (≥ large) (Table 2), presence of flatulence (Table 3). Cats were usually fed dry pet food, but not dietetic digestive food in the last month.
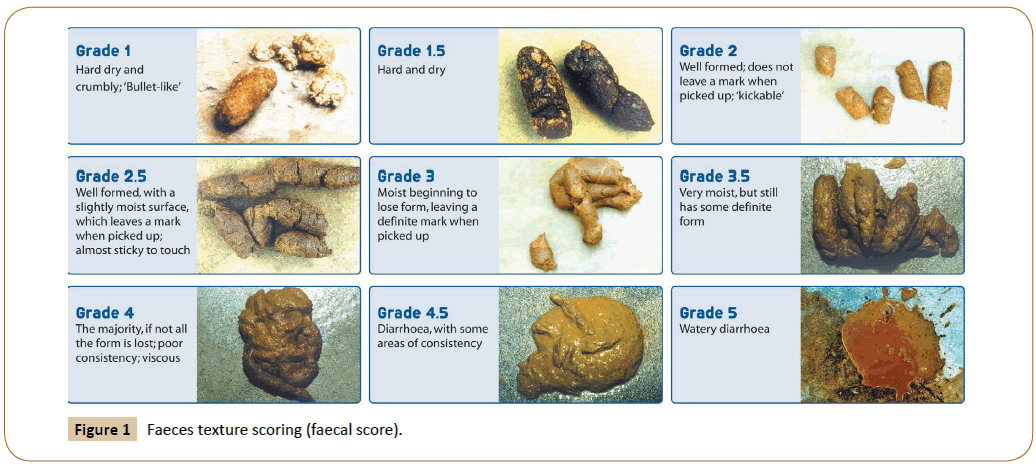
Figure 1: Faeces texture scoring (faecal score).
| Very slightly odorous (very acceptable) |
Normal |
| Slightlyodorous (acceptable) |
| Mildlyodorous (slightly acceptable) |
| Odorous (slightlybearable) |
Abnormal |
| Veryodorous (unbearable) |
Table 1: Faeces odour scoring.
| Verysmall |
Normal |
| Small |
| Medium |
| Large |
Abnormal |
| Very large |
Table 2: Faeces quantity scoring.
| Never |
Normal |
| Sometimes |
Abnormal |
| Often (several times a week) |
| Very often (several times a day) |
Table 3: Flatulence frequency scoring.
Test diet
The test diet was a new dry diet intended for the management of chronic maldigestion-malabsorption in cats (Table 4). It was formulated to provide complete nutrition and to be highly digestible. Regarding the macronutrient profile, the diet was a high protein – low carbohydrate – high fat diet. By addition of fish oil, the diet had an increased level of omega-3 fatty acids, in order to help reduce excessive inflammation as described in literature. According to ref. [17,18] the diet was also supplemented in various functional ingredients known for their complementary beneficial actions on GI health: fructo-oligosaccharides, psyllium fibre, nucleotides, beta-glucan, pasteurised Lactobacillus acidophilus, and butyrate. Added butyrate was protected by coating to allow gradual release over the intestinal tract. Coating was also aimed to reduce the typical unpleasant smell of butyrate.
Metabolisable Energy (measured in vivo) (kcal/100g)
Protein (% ME)
Fat (% ME)
Carbohydrate (% ME)
Crude cellulose (% DM)
Soluble fibre (% DM)
Insoluble fibre (% DM)
Total omega-6 fatty acids (% DM)
Total omega-3 fatty acids (% DM)
Apparent digestibility coefficient of protein (%) (in vivo)
Apparent digestibility coefficient for fat (%) (in vivo) |
419
39
45
16
3.7
1.6
7.9
3.7
1.1
86
91 |
Composition: Pork and poultry dehydrated protein, potato starch, animal fat, whole pea, mineral salts, pork and poultry hydrolysed protein, beet pulp, lignocellulose, linseed, fish oil, psyllium fibre, fructo-oligosaccharides, chitosan, yeast nucleotides, yeast beta glucan, butyrate salts, pasteurised Lactobacillus acidophilus.
Table 4: Nutritional characteristics of the test diet=Virbac VETERINARY® HPM Digestive Support Cat (ME=metabolisable energy, DM=dry matter).
The test diet was provided in neutral bags, pet owners had no information about the brand, the composition and the nutrient profile. The only information given to pet owners was the feeding table which precised the daily quantity of kibbles to maintain their cats at optimal body weight.
Study design
Cats were followed up for two months. During the first month (M1), after a 4-day diet transition, they were fed exclusively the test diet. During the second month (M2), they were fed again their usual dry diet. No medical management was allowed during the study; if medical treatment became necessary, the cat was excluded.
For assessment, pet owners had to fill in online multiple-choice questionnaires. By individual phone meetings at the beginning of the study, pet owners confirmed their commitment and their understanding of all the items included in the questionnaires. Assessments were performed 6 times: at inclusion (=basal assessment with usual diet), then each week of M1, and finally at the end of M2. The 5 digestive parameters previously defined were assessed to describe the cat’s clinical status. Owners had then to compare parameters with previous assessment and basal assessment in order to describe their cat’s status improvement or degradation. Owners answered also questions about kibbles characteristics, palatability, and general satisfaction. They were asked to give a satisfaction score from 0 (not satisfied at all) to 10 (totally satisfied) and precise strengths and weaknesses of the tested product.
Data analysis
At each time, mean frequency of defecation and mean faecal score were calculated by averaging all the corresponding individual figures. Wilcoxon signed rank and Mc Nemar’s tests were performed to compare each parameter at different times, with a significant threshold of 5%.
Results and Discussion
Three cats did not complete the study. One cat was removed because of poor palatability and consumption of the test diet. Two cats were lost during the second month of the study. So, 44 cats were analyzed. Cats were aged from 0.7 to 8 years (mean age: 3.5 ± 2.6). None of the cats required medical treatment during the study. Therefore it is assumed that results reflected the only effect of the dietary management. Initial mean body weight and body condition score (nine-point system) averaged 4.2 ± 1.6 kg and 5.3 ± 0.6, respectively, with no significant change throughout the study.
Regarding the design of the study and the analysis of the following results, a potential limit was the absence of randomization and control group, comparing the results of one group fed the test diet and one group fed a reference diet (commercially available therapeutic pet food intended for the management of gastrointestinal disease in cats). In this study, the design supposed that the usual diet could be the control diet, and that each cat could be its own control since fed successively with the two diets.
Frequency of defecation
The mean frequency of defecation significantly decreased from 3.2 ± 0.8 at inclusion to 2.1 ± 0.6 at the end of M1 (p<0.0001), and then increased to 2.8 ± 0.8 at the end of M2 with the usual diet (p<0.0001) (Figure 2). The decrease was significant as soon as the first week of M1 (p<0.0001). Out of the 39 cats having « abnormal » frequency of defecation at inclusion, 34 cats improved when fed the test diet, and 22 of them degraded again when switched to their usual diet. Degradation was quick, observed within the 2 first weeks for all these cats. Consequently, the rates of cats with « normal » frequency of defecation significantly changed between the 3 time points (Table 5): at the end of M1, 80% of cats had a « normal » frequency of defecation, compared to 15% at inclusion and 41% at the end of M2.
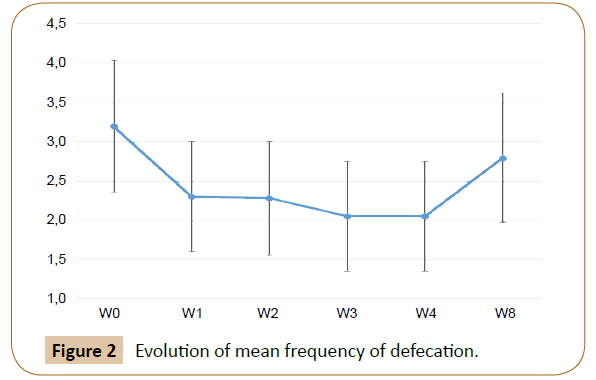
Figure 2: Evolution of mean frequency of defecation.
| Digestive parameter |
Considered as «normal» when: |
Cats (%) with«normal»parameter |
| Inclusion |
End of M1 |
End of M 2 |
| Frequency of defecation |
≤ 2 times/day |
15 |
80*** |
41*** |
| Faecal score |
≤ 2.5 |
43 |
91*** |
66** |
| Faecesodour |
≤mildlyodorous |
0 |
85*** |
50*** |
| Faecesquantity |
≤ medium |
65 |
100** |
77* |
| Frequency of flatulence |
never |
41 |
98*** |
91NS |
Table 5: Percentage of cats with «normal» parameters at different time points, Comparison «End of M1» vs «Inclusion», and «End of M2» vs «End of M1»: NS (non significant), *: p≤0.05, **: p≤0.001, ***: p≤0.0001.
Faecal score
The mean faecal score significantly improved from 3.1 ± 0.7 at inclusion to 2.3 ± 0.4 at the end of M1 (p<0.0001), and then degraded to 2.7 ± 0.6 at the end of M2 with the usual diet (p<0.0001) (Figure 3). The improvement was significant within the first week of M1 (p<0.0001). Out of the 26 cats having « abnormal » faecal score at inclusion, 24 cats improved during M1, and 13 of them degraded again during M2. Table 5 shows the significant changes in the rates of cats with « normal » faecal score: at the end of M1, 91% of cats had a « normal » faecal score, compared to 43% at inclusion and 66% at the end of M2.
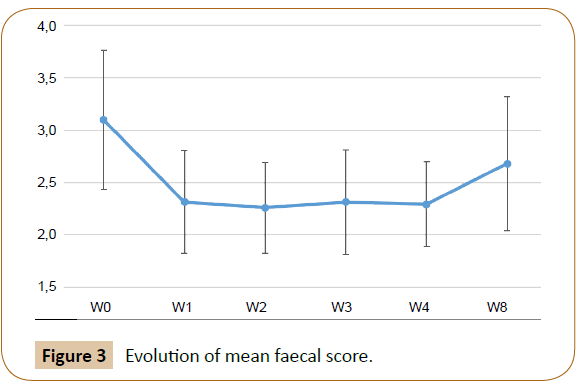
Figure 3: Evolution of mean frequency of defecation.
Faeces odour
At inclusion, all owners considered that their cats had « abnormal » stool odor (Table 5). Forty-two cats improved when fed the test diet, and 32 of them degraded again when switched to their usual diet. At the end of M1, 85% of cats were considered as « normal » for this parameter. At the end of M2, the rate decreased to 50%.
Faeces quantity
When considering faeces quantity, a decrease was observed and at the end of M1, all cats (100%) had this parameter « normal » when changed back to their usual diet (Table 5), 22 owners observed an increase in their cat’s faeces quantity, and 77% cats were considered « normal » at the end of M2.
Frequency of flatulence
Regarding flatulence parameter, 41% of cats were considered as « normal » at inclusion because they never presented flatulence (Table 5). When feeding cats with the test diet, a significant improvement was observed since 98% of cats had no flatulence during M1. This parameter did not significantly changed during M2.
During M1, none of the 5 parameters were degraded in cats, parameters were unchanged, improved, or cured (i.e., improved and become normal). Improvement was very quick in almost all cats: depending on the parameter, 81 to 96% of responder cats did improve as soon as the first week fed the test diet (82% for frequency of defecation, 96% for faecal score, 95% for faeces odor, and 81% for faeces quantity). Finally, 72% of cats were completely “cured” (all parameters normal) after 1 month fed the test diet, 26% were partially “improved” (some parameters unchanged, some improved but still abnormal, and some become normal), and only 2% (one cat) were “unchanged” (Figure 4).
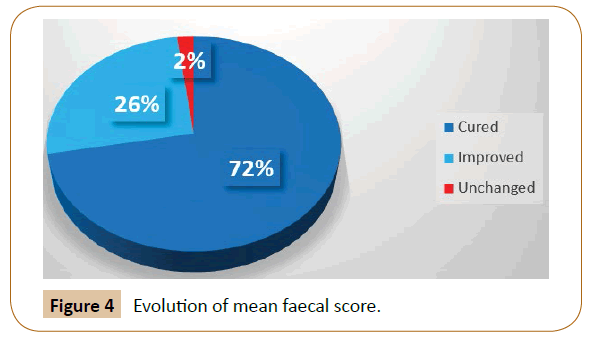
Figure 4: Evolution of mean faecal score.
On the contrary, the switch to usual diets during M2 resulted in degradation of the digestive status for most cats: at the end of M2, 61% of cats had minimum 1 parameter degraded again.
Palatability
At the end of M1, 89% of owners considered that their cats appreciated the test diet, and 55% précised that their cats preferred the test diet compared to their usual diet. The high level of palatability may be explained by the high part of ingredients from animal origin, in respect of carnivore’s preference: poultry fat and fish oil as the only sources of fat, pork and poultry protein as the main source of protein (94% of total protein).
General satisfaction
Combining all the assessed parameters, 85% of owners declared to be satisfied by the test diet. The mean satisfaction score was 8.0 ± 1.8. The most commonly cited strengths were the high palatability, the improvement in the digestive status, and the adapted size and shape of the kibbles. Forty-three per cent of pet owners said that they did not notice any weakness. The most common cited weakness was the strong odor of the kibbles when opening the bag. This odor could be partly explained by the supplementation in butyrate. Despite a specific coating, the smell of butyrate was not completely masked. It is interesting to notice that the strong smell for pet owners did not impact the palatability in cats.
Conclusion
Although this study did not contain a control group, the results confirmed that the new highly digestible diet with high protein - low carbohydrate - high fat levels and specific supplementation in digestive functional ingredients was beneficial in the management of feline chronic gastrointestinal disease. Clinical improvement was quick and significant. The switch to usual diets resulted in the degradation again of the digestive status of the cats, suggesting that the new diet may also be proposed in a longer term for the prevention of recurrences in cats subject to digestive disorders.
References
- Guilford WG (1994) Nutritional management of gastrointestinal tract diseases of dogs and cats. J Nutr 124: 2663S-2669S.
- Kirk CA (2007) The use of long chain omega-3 fatty acids in inflammatory bowel disease. Proceedings of the NAVC Congress, Orlando, Florida.
- Davenport DJ, Jergens AE, Remillard RL (2010) Inflammatory bowel disease. Small Animal Clinical Nutrition. 5th edn. Mark Morris Institute,USA, pp: 1065-1074.
- Davenport DJ, Remillard RL, Simpson KW (2010)Exocrine pancreatic insufficiency. In: Small Animal Clinical Nutrition. 5th edn. Mark Morris Institute,pp: 1135-1141.
- Zoran DL (2008) Nutritional management of feline gastrointestinal diseases. Top Comp Anim Med 23: 200-206.
- Laflamme DP, Xu H,Long GM (2011) Effects of diets differing in fat content on chronic diarrhoea in cats. J Vet Intern Med 25: 230-235.
- Sparkes AH, Papasouliotis K, Sunvold G (1998) Effect of dietary supplementation with fructo-oligosaccharides on fecal flora of healthy cats. Am J Vet Res 59: 436-440.
- Kanakupt K, Vester BBM, Dunsford BR, Fahey GC (2011) Effects of short-chain fructo-oligosaccharides and galacto-oligosaccharides, individually and in combination, on nutrient digestibility, fecal fermentative metabolite concentrations, and large bowel microbial ecology of healthy adults cats. J Anim Sci89: 1376-1384.
- Hamer HM, Jonker D, Venema K (2008) Review article: the role of butyrate on colonic function. Aliment Pharmacol Ther27: 104-119.
- Guilloteau P, Martin L, Eeckhaut V (2010) From the gut to the peripheral tissues: the multiple effects of butyrate. Nutr Res Rev 23: 366-384.
- Paap P (2014) Butyrate and its multifarious effects. AllAboutFeed 22: 23-25.
- Gross KL, Yamka RM, Khoo C (2010) Chapter 5: Macronutrients. In: Small Animal Nutrition. 5th edn. Mark Morris Institute,USA,pp: 49-105.
- Bueno J, Torres M, Almendros A (1994)Effect of dietary nucleotides on small intestinal repair after diarrhoea. Histological and ultrastructural changes. Gut35: 926-933.
- Carver JD (1994) Dietary nucleotides: cellular immune, intestinal and hepatic system effects. J Nut 124: 144S-148S.
- Fontana L, Martinez-Augustin O, Gil A (2010) Role of dietary nucleotides in immunity. Functional Food Review 2: 1-10.
- Carretero MI, Pozo M (2010) Clay and non-clay minerals in the pharmaceutical and cosmetic industries. Part II. Active ingredients. Applied Clay Science 47: 171-181.
- Moxham G (2001) The Waltham Faeces Scoring System - A tool for veterinarians and pet owners: how does your pet rate? Waltham Focus 11: 24-25.
- Bauer JE (2011) Therapeutic use of fish oils in companion animals. J Am Vet Med Assoc 239: 1441-1451.